Nobody fully prepares you for what your body feels like after birth. You knew it would be hard. You knew things would change. But standing in the bathroom a few days postpartum, looking in the mirror, wearing a diaper-sized pad and leaking colostrum through your shirt — that moment has a particular quality that no amount of reading quite gets you ready for.
Your body just did something extraordinary, and it is now in the middle of one of the most significant physical transitions it will ever go through. Some of what happens will resolve in days. Some will take months. Some changes will be permanent. All of it is worth understanding — not so you can control the process, but so you can stop wondering whether what you’re experiencing is normal.
This guide covers what actually happens to your body after birth, from the first week through the first year and beyond — week by week, system by system, honestly.
The Fourth Trimester: What It Actually Is
The first three months after birth are increasingly recognized as a distinct phase — the “fourth trimester” — a time of profound physical and emotional adjustment that deserves as much attention as the pregnancy itself. ACOG has pushed for this framing precisely because postpartum care has historically been reduced to a single six-week checkup, which misses most of what actually happens in the months following birth.
During this time your uterus is shrinking, your hormones are crashing, your body is either establishing or suppressing milk production, your wounds are healing, and your sleep is being fragmented in ways that affect every physiological system. Understanding what’s happening and why is what allows you to take it seriously rather than pushing through it alone.
The First Week: The Most Dramatic Physical Changes
What Happens to Your Uterus
Within minutes of delivering the placenta, your uterus begins contracting back toward its pre-pregnancy size — a process called involution. Immediately after birth it weighs about 2.5 pounds and extends to your navel. By one week, it has shrunk to roughly 1 pound and is halfway to the pubic bone. By six weeks, it returns to its pre-pregnancy weight of approximately 2 ounces.
The contractions that drive this process — called afterpains — are noticeable, and the Mayo Clinic notes they’re typically stronger in women who have had previous pregnancies and most intense during breastfeeding (because nursing triggers oxytocin, which drives uterine contractions). This is biology doing something useful, even when it hurts.
Vaginal Bleeding (Lochia): What’s Normal
Lochia is the postpartum discharge of blood, mucus, and uterine lining — and it’s heavier than most women expect. In days 1 to 5, bleeding is bright red and similar in flow to a heavy period, possibly with small clots. From days 5 to 14, it transitions to a pinkish or brownish discharge with lighter flow. From weeks 2 to 6, discharge becomes yellowish-white and gradually tapers.
Clots smaller than a grape are normal. Soaking a pad in an hour, or clots larger than a golf ball, are not — those need a call to your provider that day. Flow increases with activity and breastfeeding; a rush of blood when you stand from lying down is just pooled blood releasing, not a cause for alarm on its own. The full picture of what postpartum body changes look like week by week is in the guide to postpartum body changes in the first 6 weeks.
Perineal Healing
If you delivered vaginally, your perineum — the area between the vagina and anus — will be sore, swollen, and possibly bruised. If you had a tear or episiotomy, stitches are present but dissolve on their own over 2 to 3 weeks. Ice packs help the first 24 to 48 hours; warm sitz baths help after that. Using a peri bottle with warm water during bathroom visits significantly reduces stinging from stitches. Sitting may be uncomfortable for the first week.
The Belly After Birth
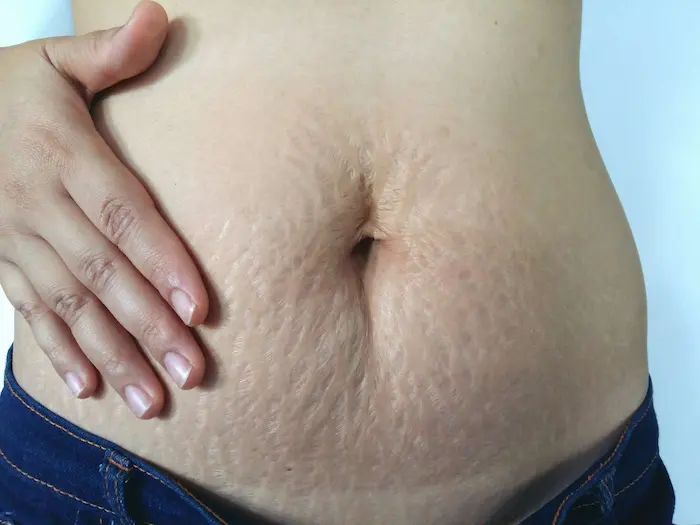
Your belly will still look significantly pregnant immediately after birth. The skin is stretched, the muscles are separated, there’s still fluid and expanded organs. This is not a failure of anything — it’s what a body looks like after nine months of growing a person. Over the coming weeks your abdomen will gradually decrease in size as the uterus contracts, retained fluid is shed, and tissues begin to reorganize. The timetable for the belly after birth is measured in months, not days.
Breast Changes in the First Week
In the first few days, your breasts produce colostrum — a thick, yellowish, concentrated fluid packed with antibodies and exactly what your newborn’s immature gut needs. Around days 3 to 5, milk “comes in” and breasts become full, firm, warm, and often painful — engorgement. This is the most intense breast experience of the postpartum period. Nursing or pumping frequently is the most effective relief; cold packs between feeds help inflammation; warm compresses before a feed encourage milk flow. Engorgement typically resolves within a week to ten days as supply and demand calibrate.
Weeks 2 to 6: Active Healing
Weight Changes After Birth
Most women lose 10 to 12 pounds immediately after birth — baby, placenta, and amniotic fluid. In the weeks that follow, additional weight drops as the body sheds retained fluid; postpartum night sweats are partly the body eliminating this excess water through sweat. The CDC notes that gradual, steady weight loss is healthier than rapid loss, particularly for breastfeeding mothers. Postpartum weight loss follows its own timeline for every woman and is not well-served by urgency.
Skin Changes
Stretch marks, if they appeared during pregnancy, may initially look more vivid as the skin deflates. They typically fade from red or purple to silvery-white over 6 to 12 months. The linea nigra — the dark line down the pregnant belly — usually fades within months. Melasma (darkening of facial skin sometimes called the “pregnancy mask”) generally lightens postpartum as estrogen levels drop. Varicose veins may improve as pressure on pelvic veins decreases.
Hair Shedding
Around 3 to 4 months postpartum, many women lose large amounts of hair — sometimes in alarming clumps. This is not hair loss in the clinical sense; it’s telogen effluvium. During pregnancy, high estrogen levels kept hair in the growth phase longer than usual. After delivery, when estrogen drops sharply, all that extra hair sheds at once. The American Academy of Dermatology confirms this is temporary and normal. Regrowth follows, sometimes with a different texture or wave pattern than before. If shedding continues past 6 months or you notice distinct bald patches, a dermatologist visit is worthwhile.
Foot Changes
Some women permanently go up half a shoe size or more after pregnancy. Relaxin — the hormone that loosened pelvic ligaments for birth — also affects foot ligaments, allowing the bones to spread and the arch to flatten slightly under the increased weight of pregnancy. For some women this is temporary; for others, the change is permanent. If your pre-pregnancy shoes feel tight a year postpartum, they probably are.
Months 2 to 6: The Adjustment Phase
When Your Period Returns
For formula-feeding mothers, menstruation typically returns 6 to 12 weeks postpartum. For breastfeeding mothers, the timeline varies considerably — anywhere from 3 months to 18 months or longer, depending on how frequently and exclusively you’re nursing. Prolactin, the milk-producing hormone, suppresses ovulation — which is why breastfeeding delays the period but is not reliable contraception. Ovulation can return before your first postpartum period, meaning you can conceive without warning.
When your period does return, the first few cycles may be heavier, more painful, or less regular than they were before pregnancy. This typically normalizes over time.
Abdominal Muscles and Diastasis Recti
The rectus abdominis muscles — the ones that run vertically down the front of your abdomen — separate to accommodate the growing uterus. This happens to some degree in most pregnancies. When the gap doesn’t close adequately after birth, it’s called diastasis recti, and it affects how the core functions.
You can check for it: lie on your back with knees bent, lift your head and shoulders slightly, and feel above and below your navel for a gap between the muscle bellies. More than two fingerbreadths is significant. If you have diastasis recti, standard core exercises like crunches actively make it worse — the guide to diastasis recti recovery explains what actually helps.
Pelvic Floor Changes
The pelvic floor — the group of muscles that support the bladder, uterus, and bowel — bears the full weight of pregnancy and the significant strain of labor and delivery. Common postpartum experiences include leaking urine when coughing, sneezing, or exercising; a feeling of heaviness or pressure in the pelvis; and decreased sensation during intercourse. The WHO recognizes pelvic floor dysfunction as a common postpartum condition that deserves treatment, not just acceptance. Pelvic floor physical therapy is the evidence-based approach — and it’s never too late to start. Everything you need to know about postpartum pelvic floor recovery is worth reading if any of this sounds familiar.
Scar Healing
C-section and episiotomy scars continue maturing well past the first weeks. Redness fades over months. Scars flatten and soften. Numbness or tingling around the incision site may persist for months as nerves regenerate — this is normal and typically resolves, though it can take a year. Gentle scar massage (once the incision is fully closed and provider-approved) can help prevent adhesions that affect how the surrounding tissue moves. C-section internal healing takes significantly longer than external healing suggests — the C-section recovery timeline is worth understanding if that was your delivery.
Months 6 to 12: Finding a New Normal
Weight and Body Composition
Most women reach a stable weight somewhere between 6 and 12 months postpartum. But weight alone tells an incomplete story. Even at the same number on the scale, your body composition may be different — more fat in different places, less muscle, different distribution. Many women notice permanently wider hips (pelvic bones can shift), different fat distribution, changed breast shape, and a softer abdominal contour that reflects changed muscle structure rather than just excess weight. These aren’t problems to fix — they’re what a body that has been through pregnancy looks like.
Thyroid Function
Some women develop postpartum thyroiditis in the months after birth — an inflammatory condition that can cause the thyroid to swing from overactive to underactive. Because the symptoms (fatigue, mood changes, weight changes, temperature sensitivity) look so similar to normal new-parenthood experiences, it’s frequently missed. If fatigue seems disproportionate to your sleep situation, or if other thyroid symptoms are present, ask your provider specifically for a thyroid panel. The full picture of postpartum thyroid issues explains what to watch for and when to push for testing.
Breasts After Breastfeeding: What Actually Happens
The breast changes of breastfeeding extend through nursing and beyond weaning. During active breastfeeding, breasts fluctuate significantly in size and feel depending on timing — very full before a feed, noticeably softer after. Breasts feeling less full between feeds around weeks 4 to 6 is a sign of supply regulation, not a drop in milk — a distinction worth knowing before you panic and assume you’re losing supply.
Plugged ducts feel like tender lumps and need to be resolved promptly — continued nursing and gentle massage are first-line approaches. If a plugged duct develops into mastitis (fever, flu-like symptoms, one area of the breast that’s red and hot), the AAP recommends continuing to nurse through it and seeking antibiotics. The bacterial infection is in the breast tissue, not the milk, and nursing is both safe for baby and helps clear the duct.
After weaning, breasts go through another transition. Many women find their breasts are smaller or deflated-looking, less full, or differently shaped than before pregnancy — often attributed specifically to breastfeeding, though most breast shape changes come from the pregnancy itself rather than the nursing. Genetics, age, and how many times you’ve been pregnant all influence outcomes more than the specific feeding choice. Supporting the breasts well during and after nursing helps, but there’s no intervention that prevents all change.
Postpartum Body Changes That Often Go Unmentioned
Joint and Ligament Changes
Relaxin stays in your system for months after birth, continuing to affect joint stability even after you’ve delivered. This is why the postpartum period carries elevated injury risk during exercise — joints that are more flexible than usual are also more vulnerable. Back pain is common from the combination of carrying baby, nursing posture, and the still-altered joint landscape. Gentle movement and attention to body mechanics help. Avoid high-impact exercise before the pelvic floor and core have been properly rehabilitated.
Night Sweats and Temperature Regulation
Postpartum night sweats are common and can be dramatic — soaking sheets, waking you even on top of the already fragmented sleep from the baby. This is the body eliminating the extra fluid it retained during pregnancy and reflects the dramatic hormonal shift after delivery. Breathable sleepwear, light bedding, and staying hydrated all help. It typically resolves within a few weeks. The full explanation for why this happens is part of postpartum hormonal changes.
Swelling
Many women are surprised that postpartum swelling can be more significant than pregnancy swelling. Your body is shedding the enormous amount of extra fluid pregnancy required, and that process takes time. Swollen ankles and feet at the end of the day, puffy hands and face upon waking, rings that won’t go on — all common in the first week or two. Elevating feet, staying hydrated, gentle movement, and compression socks help. If swelling is severe, only in one leg, or accompanied by pain, contact your provider — one-sided leg swelling can indicate a blood clot.
Vision and Dental Changes
Temporary vision changes — blurriness, difficulty with contact lenses — can occur postpartum from hormonal shifts affecting corneal shape and from fluid changes. These typically resolve without intervention, but if vision changes are sudden or severe, contact your provider. On the dental side, pregnancy gingivitis can persist postpartum; gum sensitivity, bleeding when brushing, and increased cavity risk are real concerns during this period. The CDC recommends continuing dental care postpartum — your own health appointments matter as much as your baby’s.
Nutrition for Physical Recovery
What you eat has direct effects on how your body heals. Protein — from lean meat, poultry, fish, eggs, dairy, legumes, or nuts — supports tissue repair and should anchor each meal. Iron-rich foods matter particularly if you lost significant blood during birth: red meat, dark leafy greens, fortified cereals, and legumes, all paired with vitamin C for better absorption. Calcium supports bone health depleted by pregnancy and breastfeeding; dairy, fortified plant milks, leafy greens, and canned salmon with bones are all good sources. Fiber prevents constipation, which postpartum hormonal shifts and pain medications make more likely; whole grains, fruits, vegetables, and legumes help alongside adequate hydration.
Hydration deserves special attention — if you’re breastfeeding, your fluid needs are significantly elevated. The simplest practice: drink something every time you sit down to nurse. Keep a water bottle wherever you feed the baby. Your body is doing a lot right now and it needs fuel to do it. The full guide to postnatal nutrition gives specific guidance on eating well during this season.
Returning to Exercise
In the first weeks: gentle walking, pelvic floor contractions (if comfortable), and nothing heavier than your baby. If activity increases bleeding, that’s your body telling you to do less. After provider clearance at around six weeks, movement can gradually increase — walking first, then targeted core rehabilitation (not crunches), then building from there. A pelvic floor physical therapist assessment at this point is valuable even without specific symptoms — it establishes what’s actually happening rather than guessing. The phased guide to returning to exercise after baby gives specific guidance on what each phase should look like.
Body Image and the Emotional Reality
The physical changes of postpartum are inseparable from the emotional experience of them. Many women feel genuinely unprepared for how different their bodies look and feel after birth — not because they weren’t warned, but because the warnings don’t quite capture the reality of standing in a body that doesn’t feel like yours anymore.
Social media images of rapid postpartum “bounce back” have created a cultural expectation that is both unrealistic and genuinely harmful. Most women’s bodies do not return to their pre-pregnancy shape — they build new shapes that carry the physical record of what they went through. That’s not failure. It’s what happens.
Disconnection from your body, frustration when clothes don’t fit, grief for your pre-pregnancy shape, impatience with how long healing takes — all of these are normal responses to a genuinely significant change. So is pride at what your body accomplished, and the complex ambivalence of feeling both of those things simultaneously. If body image concerns are significantly interfering with daily life, your relationship with your baby, or your basic self-care, that’s worth raising with a therapist who understands perinatal mental health. The WHO is explicit that maternal mental health is essential to overall postpartum wellbeing — not peripheral to it.
When to Call Your Provider
Most of what happens to your body after birth is normal. But certain symptoms need same-day attention: heavy bleeding soaking a pad in an hour, clots larger than a golf ball, fever above 100.4°F, severe headache that doesn’t respond to medication (especially with vision changes), chest pain or difficulty breathing, swelling or pain in one leg, redness or discharge from an incision, painful or difficult urination, or severe abdominal pain.
On the emotional side: persistent sadness or emptiness that isn’t improving, inability to bond with your baby, thoughts of harming yourself or your baby, overwhelming anxiety or panic attacks, or difficulty caring for your own basic needs all warrant reaching out to your provider promptly rather than waiting to see if they resolve. Knowing what’s a warning sign versus what’s an expected part of postpartum adjustment is also covered in the guides to postpartum depression signs and when to seek postpartum help.
Frequently Asked Questions
How long does it take for the belly to go down after birth?
Significantly but not completely in the first few weeks, as the uterus shrinks and retained fluid is shed. Many women still have a visible soft belly or “pooch” at 3 months, and full abdominal recovery — to the extent it happens at all — often takes 6 months to a year or longer. For women with significant diastasis recti, the timeline with proper rehabilitation can extend further. The belly after birth is not on anyone else’s schedule.
Will I lose the pregnancy weight?
Many women lose most of the pregnancy weight within 6 months, though this varies significantly. But weight as a single number misses most of the picture — body composition, shape, and where weight is distributed all change with pregnancy in ways that weight alone doesn’t capture. What matters more than a number is whether you feel strong, well-nourished, and able to do what you want to do. Focusing on health and function rather than a specific weight tends to produce better outcomes, physically and mentally.
Why am I still leaking urine when I cough or sneeze?
Stress incontinence (leaking with cough, sneeze, laugh, or exercise) is common postpartum and is a sign of pelvic floor dysfunction — not just “something you have to live with.” Pelvic floor physical therapy addresses this effectively. If leaking is still happening at 6 weeks postpartum and bothering you, bring it up at your checkup rather than assuming it’s normal. It’s common; it’s not inevitable.
Will my breasts sag after breastfeeding?
Research actually shows that breastfeeding itself doesn’t cause breast sagging — the changes happen because of pregnancy, not nursing. The expansion and contraction of breast tissue during pregnancy, weight changes, age, genetics, and number of pregnancies all play roles. Supporting the breasts well with a properly fitted bra during and after nursing helps, but there’s no intervention that fully prevents the shape changes that pregnancy creates.
Is it normal to have no sex drive postpartum?
Very normal, and for multiple overlapping reasons. Physical healing, low estrogen (especially while breastfeeding), exhaustion, changed body image, the mental load of new parenthood, and the sheer fact of being touched constantly by a baby all affect libido. Desire typically returns gradually as healing progresses and hormones stabilize, though the timeline varies widely. If low libido is persistent, distressing, or accompanied by pain with intercourse, that’s worth discussing with your provider — it’s not something you have to just wait out indefinitely.
Why do my joints hurt so much postpartum?
Relaxin remains elevated in your system for months postpartum, keeping joints looser and more vulnerable than pre-pregnancy. The physical demands of new parenthood — lifting, carrying, nursing in repetitive positions, bending repeatedly — compound this. Back pain and hip pain are particularly common. Gentle movement, attention to posture during feeding, and avoiding high-impact activity before your core and pelvic floor have been properly rehabilitated all help. If joint pain is severe or localized, a physiotherapy assessment can identify what specifically is going on.
One Last Thing
Your postpartum body is not a before-and-after. It is a body mid-process, doing a remarkable amount of work that you can’t always see or measure. Some of what it’s doing will resolve. Some of it will settle into your permanent shape. All of it is the record of what you went through to bring your child into the world.
Be patient with the process. Ask your provider about things that concern you rather than assuming they’re just something to endure. And stop asking when you’ll get your body back — you have your body right now. It’s just in the middle of something significant.
References
- American College of Obstetricians and Gynecologists (ACOG) – Optimizing Postpartum Care
- Mayo Clinic – Postpartum Care: What to Expect After Vaginal Birth
- Centers for Disease Control and Prevention (CDC) – Postpartum Health
- American Academy of Dermatology – Hair Loss During Pregnancy and After Childbirth
- World Health Organization (WHO) – Maternal Mental Health
- American Academy of Pediatrics (AAP) – Breastfeeding and the Use of Human Milk

