Let’s start with a fundamental truth: Labor involves pain. It’s the physiological signal of powerful muscles working to open a passage and bring new life into the world. But how you experience that pain—and more importantly, how you manage it—is deeply personal and full of choice. The cultural narrative often presents a false dichotomy: you either “tough it out” naturally or you “get the drugs.” This oversimplification does a disservice to every expecting parent.
The reality is that modern labor pain management is a rich spectrum, a toolkit with more options than you might realize. It’s not a linear path from “least” to “most” intervention, but a menu you can navigate based on your moment-to-moment needs, your birth philosophy, and how your unique labor unfolds.
This guide is designed to demystify that entire spectrum. We’ll walk through every major category of pain relief, from breath and water to epidurals and beyond. We’ll cover the how, the why, the pros, and the realistic considerations for each, arming you with the knowledge to create a personalized pain management plan for labor. Your goal isn’t to commit to one option at 30 weeks, but to understand your choices so you can collaborate with your birth team from a place of confidence, not fear.
Reframing the Goal: From Pain Elimination to Pain Coping
Before diving into the options, let’s adjust the mindset. For most, the goal of labor pain management isn’t necessarily to feel nothing (though that is a valid choice with an epidural). For many, the goal is to cope with labor pain effectively—to reduce suffering, maintain a sense of control, and conserve energy so you can be present for the birth of your child.
Pain in labor is not like a broken bone; it’s purposeful, it comes in waves, and it ends with a baby. Your management strategy can help you work with that process, not just fight against it.
Category 1: Non-Pharmacological & Mind-Body Techniques
These methods focus on using your body’s own resources, your environment, and your mind to manage pain. They are often used in combination and form the foundation of natural birth preparation.
1. Movement & Position Changes
This is your first and most powerful tool. Gravity and mobility are not just for comfort; they are biomechanical aids.
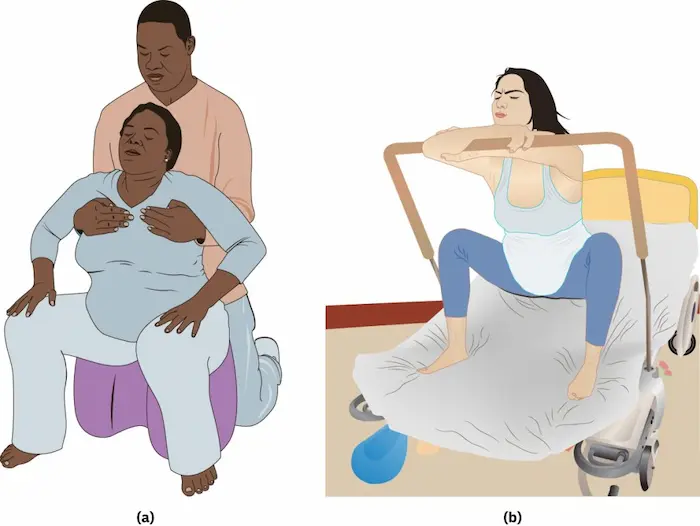
- How it Works: Upright positions (standing, swaying, slow dancing) and asymmetrical poses (lunges, hip circles on a birth ball) use gravity to help baby descend and can change the shape of your pelvis to ease pain. Using movement for labor pain relief is proactive.
- Best For: Early to active labor, anyone wanting to avoid or delay medication, and managing back labor.
- Key Consideration: Requires freedom to move, which may be limited by continuous monitoring or an epidural.
2. Hydrotherapy
Water is a remarkably effective analgesic.
- How it Works: Immersion in warm water (in a deep tub or shower) promotes relaxation, increases endorphin release, and provides buoyancy that takes pressure off joints and muscles. It can lower blood pressure and reduce the perception of pain.
- Best For: Active labor, particularly when contractions feel intense and overwhelming. The shower is great for focused back pain.
- Key Consideration: Requires access to a deep labor tub or a large shower. Some hospitals/birth centers have policies on when you can enter the water.
3. Touch & Counter-Pressure
The power of human touch should not be underestimated.
- How it Works: A doula or partner applies firm, steady pressure to your lower back/sacrum during a contraction (especially for back labor). Massage, effleurage (light stroking), and hip squeezes can interrupt pain signals and provide a focal point.
- Best For: Anyone with a support person. Essential for back labor. A core part of doula support for pain management.
- Key Consideration: Your support team needs to be taught these techniques prenatally. It can be physically demanding for them.
4. Breathwork & Vocalization
This is about channeling energy and oxygenating your body.
- How it Works: Deep, rhythmic “belly breathing” in early labor shifts to more focused, forceful breathing as intensity builds. Low moans or hums (keeping your jaw and throat loose) can help you release tension instead of holding it in your body.
- Best For: All stages of labor. It’s a portable tool you always have with you.
- Key Consideration: Practicing prenatal breathing techniques for labor makes them automatic under pressure.
5. Heat & Cold Therapy
Simple, direct sensory input.
- How it Works: A heating pad on your lower back or belly can soothe aching muscles. A cold pack on your neck or forehead can be invigorating and reduce nausea.
- Best For: Targeted relief for back pain or during pushing for perineal warmth. Cold for overheating or anxiety.
- Key Consideration: Have both options available. Never place ice directly on the skin.
6. Mindset & Distraction Techniques
Pain perception is influenced by fear and focus.
- How it Works: Hypnobirthing techniques for labor use meditation and visualization to create a state of relaxation. Focusing on a photo, mantra, or music can redirect your brain’s attention.
- Best For: Those who practice prenatally. Excellent for early labor at home.
- Key Consideration: Requires practice to be effective in active labor.
Category 2: Pharmacological & Medical Options
These involve medications to reduce or eliminate pain sensation. They are typically administered in hospital settings.
1. Nitrous Oxide (Laughing Gas)
A self-administered, inhaled option growing in popularity in the US.
- How it Works: You hold a mask and inhale a 50/50 blend of nitrous and oxygen during a contraction. It doesn’t eliminate pain but takes the “edge off,” reduces anxiety, and can create a feeling of dissociation. It leaves your system quickly when you stop breathing it.
- Pros: You control it. No effect on baby. Doesn’t slow labor. Allows full mobility.
- Cons: Can cause dizziness or nausea. May not be strong enough for transition. Not all hospitals offer it.
- Key Term:
benefits of nitrous oxide during labor
2. Opioid Analgesics (IV/IM Medications like Fentanyl, Nubain)
Systemic medications given through an IV or injection.
- How it Works: These drugs alter your brain’s perception of pain and can induce drowsiness, allowing rest between contractions.
- Pros: Can provide significant relief for those not yet ready for an epidural. Works relatively quickly.
- Cons: Crosses the placenta. Can cause drowsiness, nausea, or itching in mother and baby. May temporarily affect newborn breathing and feeding reflexes. Relief is often partial.
- Key Consideration: Timing is critical; usually not given too close to delivery to minimize infant effects.
3. Epidural Analgesia
The gold standard for complete pain relief in labor.
- How it Works: Local anesthetic (and sometimes an opioid) is delivered via a tiny catheter into the epidural space in your lower back, numbing the nerves from the abdomen down.
- Pros: Most effective pain relief available. Allows you to rest and be alert. Can be adjusted (sometimes turned down for pushing).
- Cons: Is a medical procedure with risks (headache, low blood pressure, fever). Confines you to bed, often requiring a bladder catheter. May lengthen the pushing stage and increase chance of instrumental (vacuum/forceps) delivery. May cause itching or shivering.
- Key Terms:
epidural procedure and side effects explained,walking epidural vs traditional epidural
4. Spinal Block & Combined Spinal-Epidural (CSE)
Often used for Cesarean sections or for very rapid relief.
- How it Works: Similar medication is injected directly into the spinal fluid for immediate, dense numbness. A CSE gives immediate spinal relief with an epidural catheter left in place for ongoing pain management.
- Pros: Immediate, complete relief. CSE offers the benefits of both.
- Cons: Spinal is one-time dose; can’t be topped up. Same side effect profile as epidural.
How to Make Your Choices: Building Your Flexible Plan
Your pain management plan should be a preference list, not a rigid contract. Here’s how to think it through:
- Educate Yourself: Take a comprehensive childbirth education class covering all pain relief options. Knowledge dispels fear.
- Know Your “Why”: Is your primary goal to be fully mobile? To avoid medication effects on the baby? To ensure maximum relief so you can be mentally present? There’s no wrong answer.
- Consider Your Labor Context: An induction with Pitocin often leads to more intense, painful contractions, which may influence your choices. A fast labor might leave less time for certain options.
- Practice the Non-Pharmacological Tools: Even if you plan an epidural, practice breathing and movement. You’ll use them in early labor and if there’s a delay in getting the epidural.
- Communicate with Your Provider: Discuss your preferences at a prenatal visit. Ask: “At what point in labor is it ‘too late’ for an epidural here?” “Do you offer nitrous oxide?”
- Employ a Doula: Research consistently shows that continuous labor support (a doula) reduces the use of pharmacological pain relief and increases satisfaction. They are experts in the non-pharmacological toolkit.
Navigating Common Scenarios & Questions
Q: Can I change my mind?
A: Absolutely. This is the most important point. Planning for natural birth but asking for an epidural after hours of back labor is a wise adjustment, not a failure. Planning for an epidural but finding you’re coping well is also fine. Give yourself grace.
Q: What if I have an epidural and then labor stalls?
A: This is a possibility. Your care team may recommend Pitocin to strengthen contractions. Changing positions with a peanut ball can also help progress. It’s a reason to discuss with your provider if waiting until you are 5-6 cm dilated for the epidural is appropriate for you.
Q: Are there options to help with back labor specifically?
A: Yes. Counter-pressure is the MVP. Also, hands-and-knees position, pelvic rocks, and the double-hip squeeze. Epidurals are also very effective for back pain relief.
Q: How do I know when it’s the “right time” for an epidural?
A: There’s medical timing and emotional timing. Medically, you typically need to be in active labor (4-5 cm). Emotionally, the “right time” is often when you feel you cannot cope with the current tools and need more help. Trust your instinct and your team’s assessment.
Conclusion: Your Comfort, Your Choice, Your Power
Pain management in labor is not a test of endurance. It is a series of tools to help you have a safe, positive, and empowered birth experience. The most effective plan is an informed and flexible one.
You might use the shower for hours, then get an epidural to sleep. You might use nitrous oxide through transition. You might find that movement, breath, and your partner’s touch are all you need. All these paths are valid and can lead to a beautiful, satisfying birth.
Walk into your birth knowing your options. Pack your toolkit—your breath, your movement, your knowledge, and your support team. Then, in each moment, choose what brings you comfort and confidence. That is the ultimate form of strength. You’ve got this.

