In the flurry of activity that follows birth, a quiet, profound moment occurs. Your baby is here, but they’re still connected to you by the pulsing umbilical cord. For decades, the standard practice was to swiftly clamp and cut this vital lifeline within seconds. Today, a different approach—delayed cord clamping—is changing the first minutes of life, backed by a growing body of robust scientific evidence.
This isn’t a fleeting trend, but a significant shift in understanding the physiology of newborn transition. It’s about recognizing that the umbilical cord and placenta are part of your baby’s circulatory system, not just disposable packaging. Understanding the benefits, timing, and practicalities of this simple intervention can help you have an informed discussion with your care provider and make a conscious choice for your baby’s first moments.
The Physiology: What Happens in Those First Minutes?
To understand why delayed clamping matters, we need to follow the blood. At birth, about one-third of your baby’s blood volume is still in the placenta and umbilical cord. This is not “extra” blood; it’s rightfully theirs.
When your baby takes their first breath, a miraculous cardiovascular shift occurs. Their lungs expand, and blood begins to flow to this new organ. The placenta, meanwhile, continues to pulse, transfusing this remaining blood to the baby. This process:
- Increases the baby’s blood volume and red blood cell count.
- Provides a rich infusion of iron, stored in those red blood cells.
- Transfers vital stem cells and immune factors.
Immediate clamping interrupts this physiological process. Delayed clamping allows it to complete naturally. It’s less an “intervention” and more an act of supporting natural newborn transition after birth.
The Evidence-Based Benefits: Why It Matters
Major health organizations worldwide—including the World Health Organization (WHO), the American College of Obstetricians and Gynecologists (ACOG), and the American Academy of Pediatrics (AAP)—now recommend a delay of at least 30 to 60 seconds for all healthy newborns. The benefits are well-documented:
- Improved Iron Stores for the First Year of Life: This is the most significant and well-established benefit. The iron transferred during delayed clamping increases the baby’s iron stores (ferritin levels). Adequate iron is critical for healthy brain development and cognitive function. This can be especially impactful for infants at risk for anemia, including those born prematurely or to mothers with iron deficiency.
- Reduced Risk of Neonatal Complications: For preterm infants, delayed cord clamping is considered a standard of care. It has been shown to:
- Lower the risk of intraventricular hemorrhage (bleeding in the brain).
- Reduce the need for blood transfusions.
- Decrease the incidence of necrotizing enterocolitis (a serious intestinal condition).
- Better Cardiovascular Stability: The gradual increase in blood volume helps the baby’s circulatory system adjust more smoothly to life outside the womb, leading to more stable blood pressure and heart function in those first critical hours.
- Potential Long-Term Developmental Benefits: While research is ongoing, some studies suggest the improved iron status from delayed clamping may correlate with subtle neurodevelopmental advantages later in infancy.
Importantly, these benefits come with minimal risk for full-term, healthy infants.
Timing: How Long is “Delayed”?
The term “delayed” can be vague. Here’s a clearer breakdown:
- Immediate Clamping: < 30 seconds.
- Delayed Cord Clamping (Standard Recommendation): 30 seconds to 3 minutes. For vigorous, full-term babies born vaginally, ACOG recommends at least 30-60 seconds. Many providers and parents aim for 1-3 minutes or until the cord stops pulsing.
- Lotus Birth (Umbilical Non-Severance): This is a separate practice where the cord is not cut at all; the placenta remains attached until it dries and detaches naturally days later. This is distinct from standard delayed clamping and carries different considerations (e.g., careful handling of the placenta). This guide focuses on delayed clamping, not Lotus Birth.
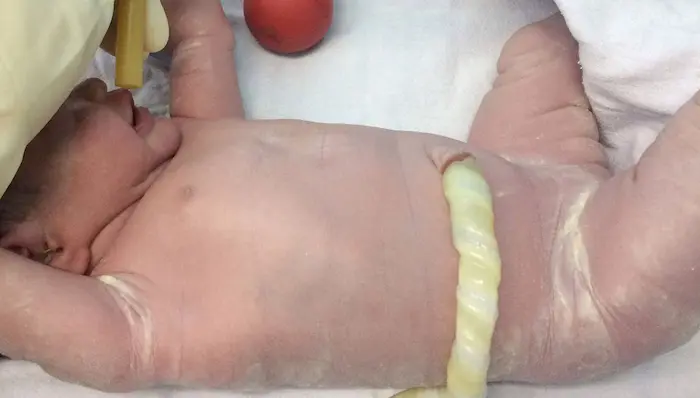
The key signal many providers use is waiting for cord pulsation to cease. When the cord goes from thick, blue, and pulsing to thin, white, and limp, the physiological transfusion is largely complete. This usually happens within 1 to 5 minutes.
Addressing Common Questions and Concerns
This practice can raise practical questions for expecting parents. Let’s address them head-on.
Q: Does delayed cord clamping increase the risk of jaundice?
This is the most common concern. The extra red blood cells do break down into bilirubin, which can cause jaundice. Research shows a slight increase in the need for phototherapy for jaundice in term infants. However, experts widely agree that the significant benefit of improved iron stores far outweighs this small, treatable risk. Jaundice is easily monitored and managed with light therapy if needed.
Q: What if I need a Cesarean section?
Delayed cord clamping is absolutely possible and recommended during Cesarean births. Your provider can lower the surgical drape for a moment, or the baby can be placed on your legs or chest while the cord is left intact for the recommended time. It requires clear communication with your OB and anesthesiologist beforehand.
Q: What if my baby needs immediate medical attention?
The recommendation for delayed clamping is for vigorous, healthy newborns. If your baby is not breathing well or needs immediate resuscitation, the NICU team’s priority will be stabilizing the baby. In some cases, they can perform initial steps (like drying and stimulating) with the cord intact. Your baby’s health always comes first, and delayed clamping is a practice for when it is safe.
Q: Can I still do skin-to-skin and breastfeed immediately?
Absolutely—and this is the ideal scenario. Delayed cord clamping does not hinder skin-to-skin contact. Your baby can be placed directly on your chest while the cord remains attached and pulsing. This combines the benefits of physiological transition with the profound bonding and newborn temperature regulation benefits of skin-to-skin. Breastfeeding can also be initiated during this time.
Q: Does it affect cord blood banking?
Yes, this is an important consideration. Collecting cord blood for private or public banking requires a sufficient volume of blood from the cord. Delayed clamping reduces the amount of blood left in the cord, which can make collection difficult or impossible. If you are planning to bank cord blood, you must discuss the trade-offs with your provider and the cord blood bank. Some banks have protocols for “partial” collections after a short delay.
How to Advocate for Delayed Cord Clamping in Your Birth Plan
Because it’s now a standard recommendation, many providers practice it routinely. However, it’s wise to ensure you’re on the same page.
- Discuss it Prenatally: Bring it up at a prenatal appointment. Say, “I’ve been reading about delayed cord clamping and understand the benefits. Is this your standard practice for healthy births?” Get their specific timing preference.
- Include it in Your Birth Plan: State it clearly and simply. For example: “For our healthy baby, we request delayed cord clamping for at least one minute, or until the cord stops pulsing, while the baby is placed skin-to-skin.”
- Communicate with Your Support Team: Ensure your partner, doula, or labor support person knows this is a priority so they can gently remind the team during the birth moment.
- Be Flexible for Safety: Reiterate that you understand this is only for a vigorous baby and that you support the medical team’s judgment if immediate care is needed.
The Bigger Picture: Integration with Gentle Birth Practices
Delayed cord clamping isn’t an isolated request; it fits seamlessly into a model of gentle, physiological birth. It’s part of a continuum that often includes:
- Immediate, uninterrupted skin-to-skin contact.
- Waiting for the baby to initiate breastfeeding cues.
- Delaying non-urgent newborn procedures (weighing, measuring, vitamin K shot) until after the first hour of bonding.
This approach prioritizes the dyad—mother and baby—as an interconnected unit during the sacred transition of birth.
A Note on “Milking” the Umbilical Cord
You may also hear about cord milking (or umbilical cord stripping). This involves manually pushing blood from the cord toward the baby before clamping. It’s sometimes used as an alternative when a full delay isn’t possible (e.g., in some emergency C-sections). For preterm infants, some studies show benefits similar to delayed clamping. For term infants, the evidence is less clear, and standard delayed clamping is the preferred, gentler method. It’s a good topic to discuss with your provider if they mention it.
Conclusion: A Simple Act with Lasting Impact
Delayed cord clamping represents a powerful return to physiological wisdom. It’s a low-tech, zero-cost practice with a high-impact payoff for your baby’s health, gifting them with a stronger nutritional foundation in their first year of life.
As you prepare for birth, you’ll make many decisions. This is one of the clearest, most evidence-based choices you can make. It requires no special equipment, just a shift in timing and perspective—a willingness to pause, observe the miracle of that pulsing cord, and allow a natural process to finish.
Have the conversation with your care provider. Add it to your birth plan. Then, in those first glorious moments after birth, as you meet your baby, you can have the peace of mind knowing you’ve already given them a vital, health-promoting gift, simply by waiting a few extra, connected minutes.

