There’s something about bringing your newborn home that makes every tiny imperfection feel monumental. So when those yellowish, crusty patches start appearing on your baby’s scalp, it’s natural to feel a wave of concern. Take a deep breath—you’re not alone, and more importantly, this is incredibly common.
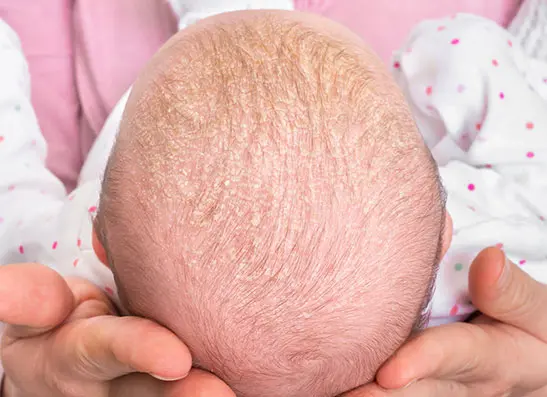
Cradle cap affects up to 70% of infants within their first three months, according to the American Academy of Pediatrics. The good news? It’s harmless, temporary, and highly manageable with the right approach. Whether you’re a first-time parent navigating postpartum life or an expectant mother preparing for what’s ahead, this guide walks you through everything you need to know about preventing and treating cradle cap.
What Exactly Is Cradle Cap? (The Medical Explanation)
Medically known as infantile seborrheic dermatitis, cradle cap isn’t an infection, a sign of poor hygiene, or an allergy. It’s simply an inflammatory skin condition that appears most frequently on the scalp—though it can occasionally show up behind the ears, on the eyebrows, or even in the diaper area.
Why Does It Happen?
The exact cause isn’t fully understood, but researchers point to a combination of factors. During pregnancy, maternal hormones cross the placenta and stimulate your baby’s sebaceous (oil) glands. After birth, those glands remain temporarily overactive, producing more oil than necessary. This excess oil traps dead skin cells, preventing them from shedding normally.
The result? Those classic cradle cap scales—yellowish, greasy, and sometimes flaky.
Additionally, a common yeast called Malassezia can sometimes colonize the oil-rich environment, potentially contributing to inflammation. The Mayo Clinic explains that while the yeast is naturally present on everyone’s skin, some infants may have a stronger reaction to it during these early months.
Is It Common in Certain Babies More Than Others?
Cradle cap doesn’t discriminate—it appears across all genders and ethnicities. However, it tends to be more noticeable in babies with darker hair, simply because the flakes contrast more visibly. Neurologically typical and medically fragile infants alike can develop it, and it has nothing to do with how often you bathe your baby or what products you use.
The condition typically emerges between two weeks and three months of age, then gradually resolves on its own within the first year. For most babies, it’s completely gone by six to twelve months.
Common Symptoms and Identification
Recognizing cradle cap is usually straightforward, but knowing exactly what you’re looking at helps distinguish it from other conditions.
What Does Cradle Cap Look Like?
The appearance can vary from mild to pronounced:
- Mild cases: Small, white or off-white flakes resembling dandruff scattered across the scalp
- Moderate cases: Thicker, yellowish, greasy-looking scales or crusts
- Pronounced cases: Dense, layered scales that may appear waxy or crusty
The underlying skin might look slightly pink or red, but generally isn’t inflamed unless irritated by scratching. Unlike some other skin conditions, cradle cap typically doesn’t itch—though if it spreads to other areas like the neck folds or behind the ears, some mild itching can occur.
Where Else Can It Appear?
While the scalp is ground zero, seborrheic dermatitis in infants can affect:
- Behind the ears: Creases may collect flaky buildup
- Eyebrows: Fine scaling along the brow ridge
- Eyelids: Rare but possible—requires extra gentleness
- Neck folds: Particularly in chubby babies with multiple skin rolls
- Armpit and diaper areas: Less common but possible
When it appears in these areas, it’s still the same condition—just in different locations. The treatment approach varies slightly based on sensitivity, which we’ll cover later.
Cradle Cap vs. Other Skin Conditions (Crucial for Parents)
One of the most common questions parents ask is whether those scalp flakes are actually cradle cap or something else entirely. Getting this right matters because treatment approaches differ.
Cradle Cap Versus Baby Eczema
This distinction trips up many parents, but there are clear differences:
| Feature | Cradle Cap | Baby Eczema |
|---|---|---|
| Appearance | Greasy, yellowish scales | Dry, red, rough patches |
| Location | Scalp, behind ears, eyebrows | Cheeks, elbows, knees, torso |
| Sensation | Usually no itching | Often intensely itchy |
| Skin feel | Oily or waxy | Dry or leathery |
The American Academy of Dermatology notes that while both conditions can coexist, they require different management strategies. Eczema typically responds to heavy moisturizers and avoiding triggers, while cradle cap responds to gentle oil treatments and regular washing.
Cradle Cap Versus Psoriasis
Infant psoriasis is much rarer than cradle cap, but it can look similar. Psoriasis plaques tend to be:
- Silvery-white rather than yellowish
- Thicker and more defined at the edges
- More likely to appear on other body parts simultaneously
If you’re unsure, a pediatrician can usually distinguish between them with a simple visual exam.
Cradle Cap Versus Baby Acne
Baby acne appears as small red bumps or pustules on the cheeks, forehead, and chin—not scales on the scalp. It’s also hormonally driven but typically resolves by four to six months without any treatment.
Step-by-Step Guide to Treating Cradle Cap at Home
Here’s where we get practical. Most cradle cap cases respond beautifully to consistent, gentle home care. The key word is gentle—aggressive scraping or picking can damage your baby’s delicate skin and potentially introduce infection.
Step 1: Softening the Scales
Trying to remove dry, stubborn scales without softening them first is like trying to scrub candle wax off a table—it doesn’t work well and risks damage.
What to use:
- Mineral oil (a classic, dermatologist-recommended option)
- Petroleum jelly (creates an effective barrier)
- Natural oils: coconut, jojoba, almond, or olive oil
How to apply:
About 15 to 30 minutes before bath time, gently massage a small amount of oil into your baby’s scalp, focusing on the areas with buildup. Use your fingertips in circular motions—no need to press hard. The oil penetrates the scales, loosening their grip on the underlying skin.
For thicker buildup, you can leave the oil on longer. Some parents apply it before a nap, then bathe the baby upon waking. Just place a soft towel under their head to protect bedding.

Step 2: Gentle Washing and Brushing
Bath time is your opportunity to gently remove those softened scales.
Washing technique:
Use a mild, fragrance-free baby shampoo. Wet your baby’s hair and scalp with warm (not hot) water, then lather the shampoo gently with your fingertips. Let the water run over the scalp to help rinse away loosened flakes.
For stubborn areas, you can use a soft-bristled brush designed specifically for babies. Many come with soft silicone bristles that are gentle enough for infant skin. Brush in gentle circles across the scalp—never scrape or pick.
What about medicated shampoos?
Some over-the-counter dandruff shampoos contain ingredients like salicylic acid or selenium sulfide. While these can be effective, the American Academy of Pediatrics advises checking with your pediatrician before using them on an infant. If recommended, they’re typically used only occasionally and rinsed immediately.
Step 3: Rinsing and Drying
Thorough rinsing matters because leftover shampoo or oil can actually worsen buildup by trapping more skin cells. Let warm water run over your baby’s scalp, gently separating hair to ensure complete rinsing.
After the bath, pat the scalp dry with a soft towel—rubbing can irritate. If you notice any loosened scales still clinging, a final gentle brush while the hair is damp can help lift them away.
Best Products and Ingredients for Treating Cradle Cap
Walking down the baby care aisle can feel overwhelming with dozens of products claiming to solve cradle cap overnight. Here’s what actually works, backed by dermatologists and pediatricians.
Medicated Options (With Pediatrician Approval)
For persistent cases that don’t respond to home care, your pediatrician might recommend:
- Ketoconazole 1% or 2% shampoo: An antifungal that targets the Malassezia yeast. Usually applied twice weekly for a few weeks.
- Selenium sulfide lotion: Helps reduce oil production and flaking. Must be rinsed thoroughly to avoid irritation.
- Salicylic acid shampoo: Helps break down scales, but use caution—it can be drying.
The Mayo Clinic emphasizes that these treatments are generally safe when used as directed, but always follow your pediatrician’s guidance on frequency and duration.
Natural and Gentle Alternatives
Many parents prefer to start with gentler options, and several have solid track records:
- Coconut oil: Contains medium-chain triglycerides with mild antimicrobial properties. It’s also deeply moisturizing and widely available.
- Jojoba oil: Closely mimics the skin’s natural sebum, making it well-tolerated and effective at softening scales.
- Shea butter: Thicker than oils, useful for very dry, stubborn patches.
- Oatmeal-based shampoos: Soothing and gentle, though less effective on thick buildup.
Brushes and Tools
A good cradle cap brush can make a significant difference. Look for:
- Extra-soft bristles: Nylon or silicone bristles that flex easily
- Small head size: Designed to fit an infant’s scalp comfortably
- Easy to clean: Sanitizing matters to prevent bacterial growth
Use the brush only on scaly areas, not on clear skin, and clean it after each use.
How to Prevent Cradle Cap from Returning
Once you’ve cleared those scales, you’ll want to keep them away. While you can’t permanently prevent cradle cap—it’s a temporary developmental phase—you can minimize recurrences.
Establish a Consistent Scalp Care Routine
The simplest prevention is regular, gentle washing. The American Academy of Pediatrics recommends washing your baby’s hair with a mild shampoo two to three times per week. This prevents oil from building up and trapping dead skin cells.
Between washes, you can:
- Gently brush the scalp daily with a soft brush to stimulate circulation and loosen any forming flakes
- Wipe the scalp with a soft, damp cloth during regular diaper changes if you notice oiliness
Pay Attention to Environmental Factors
Dry indoor air, particularly during winter months, can affect cradle cap. Using a cool-mist humidifier in your baby’s room helps maintain comfortable humidity levels that support healthy skin.
Watch for Spreading
If you notice cradle cap appearing behind the ears or in skin folds, address those areas early. A tiny amount of petroleum jelly or coconut oil applied to clean, dry skin can prevent buildup before it starts.
When to Call the Doctor: Signs of Infection or Severe Cases
Most cradle cap resolves without medical intervention. However, certain signs warrant a call to your pediatrician.
Red Flags to Watch For
Contact your healthcare provider if you notice:
- Spreading redness: Particularly if the skin looks angry, swollen, or warm to touch
- Bleeding or oozing: Scales that crack and bleed, or areas that weep fluid
- Hair loss: Though temporary hair loss can occur with heavy scaling, patchy bald spots should be evaluated
- Fever: Any fever combined with skin changes needs prompt attention
- Spreading beyond the scalp: Extensive involvement on the face, neck, or body folds
- No improvement: After several weeks of consistent home treatment
These symptoms could indicate a secondary bacterial or fungal infection requiring prescription treatment. The Centers for Disease Control and Prevention notes that while rare, infected skin needs proper medical management.
What Will the Doctor Do?
Your pediatrician will examine the affected areas and may:
- Confirm the diagnosis (often just by looking)
- Prescribe a mild hydrocortisone cream if inflammation is significant
- Recommend an antifungal cream if yeast is suspected
- Rule out other conditions if presentation is atypical
Frequently Asked Questions About Cradle Cap
Parents have questions—lots of them. Here are answers to the most common concerns.
Is cradle cap contagious?
Absolutely not. You cannot catch cradle cap from another baby, and siblings won’t develop it through contact. It’s an individual skin reaction, not an infection.
Does cradle cap bother my baby?
In most cases, no. Unlike eczema, which can keep babies awake scratching, cradle cap typically doesn’t itch or cause discomfort. The scales themselves are just dead skin—they don’t transmit sensation. However, if the area becomes inflamed or infected, discomfort can develop.
Can I prevent cradle cap during pregnancy?
There’s no proven way to prevent cradle cap before birth since it’s linked to maternal hormones and your baby’s unique skin response. However, establishing good newborn scalp care from day one can minimize severity. The American College of Obstetricians and Gynecologists emphasizes that postpartum skin care for your baby focuses on gentle cleansing regardless of whether cradle cap develops.
Will my baby lose hair?
Temporarily, yes—and that’s normal. The scales trap hair, and when they loosen, some hair comes with them. Once the cradle cap resolves, the hair grows back. Permanent hair loss from cradle cap is extremely rare.
How long does cradle cap last?
For most infants, cradle cap appears around one to three months and resolves by six to twelve months. Some babies have it only briefly; others deal with it on and off throughout their first year. Occasionally, mild dandruff can persist into toddlerhood.
Can I use adult dandruff shampoo on my baby?
Generally not recommended without pediatrician approval. Adult formulations are stronger and can be too harsh for infant skin. If your pediatrician suggests a medicated shampoo, they’ll specify which one and how often to use it.
What if it spreads to the diaper area?
Seborrheic dermatitis in the diaper area looks different from diaper rash—it’s greasier and often yellowish. Treatment involves gentle cleansing, allowing the area to air dry, and applying a protective barrier like petroleum jelly. If you’re unsure whether it’s diaper rash or seborrheic dermatitis, your pediatrician can help distinguish them.
Final Thoughts for Parents
Watching your newborn navigate any health issue, even a minor one like cradle cap, tugs at your heart in unexpected ways. You want to fix it, make it better, take it away completely. The gentle truth is that cradle cap is one of those parenting moments where patience matters more than perfection.

Your consistent, loving care—those quiet moments massaging oil into your baby’s scalp, the warm baths, the gentle brushing—all of it matters. Not just for clearing scales, but for the connection you’re building with every touch.
If you’ve tried home remedies for several weeks without improvement, or if you’re ever concerned about what you’re seeing, reach out to your pediatrician. That’s what they’re there for—to partner with you in keeping your baby healthy.
And remember, cradle cap has a 100 percent resolution rate. It will pass, your baby’s scalp will clear, and you’ll move on to the next parenting adventure, armed with a little more knowledge and a lot more confidence.

