Introduction: Your Role Is More Than Timing
Here’s a familiar scene. You and your partner have decided to try for a baby. She’s downloading ovulation apps, taking prenatal vitamins, and tracking her cycle with the precision of a NASA engineer. And you? You’re supportive, of course. You’re there for the “timed intercourse.” But privately, you might be wondering: Is that really my whole job here?
For decades, the cultural conversation around fertility has focused almost exclusively on women. But here’s the fact that changes everything: Male factors are involved in 40-50% of all infertility cases. Sometimes it’s the sole cause, often it’s a contributing factor.
This isn’t about assigning blame. It’s about claiming power. The health of your sperm is one of the most actionable variables in the conception equation. Unlike female egg quality, which is largely tied to age, you can make significant improvements to your sperm in a matter of months through targeted lifestyle changes.
As a male fertility specialist, I’ve seen the transformative impact of this knowledge. Men walk into my clinic feeling like passive bystanders on their fertility journey. They leave with a clear, empowering playbook. This guide is that playbook. We’ll cut through the noise and give you the evidence-based steps to optimize sperm health, turning you from a supportive player into a co-lead in creating your family’s future.
Sperm Health 101: What Are We Actually Optimizing?
When we talk about sperm health, we’re not just talking about quantity. It’s a multi-faceted mission. A standard semen analysis looks at four key pillars:
- Count: How many sperm are in one milliliter of semen. The World Health Organization’s lower reference limit is 16 million per mL. More is generally better, but it’s not the only factor.
- Motility: Are they swimming, and how well? We need strong, forward-moving swimmers (progressive motility) to navigate the female reproductive tract and reach the egg.
- Morphology: What shape are they? Ideally, sperm have a smooth, oval head and a long, single tail. High rates of abnormal shapes can hinder fertilization.
- DNA Fragmentation: This is the hidden factor. It measures damage to the sperm’s genetic cargo. High DNA fragmentation can lower chances of fertilization, increase miscarriage risk, and affect embryo health.
Think of it like an army. You need a good number of soldiers (count), they need to be able to march in the right direction (motility), they need the right equipment (morphology), and they need intact blueprints for building the future (DNA integrity). Your goal is to strengthen every part of this team.
The 90-Day Window: Your Timeline for Change
Here’s the single most important concept to understand: Sperm production is a 90-day project.
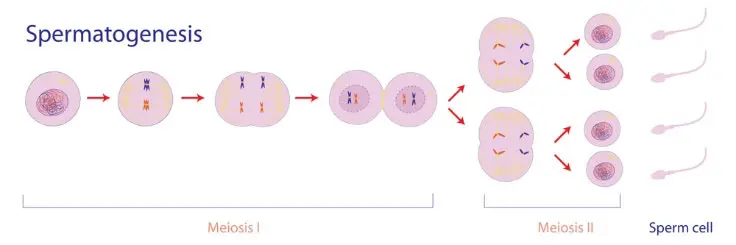
The process of creating a single sperm cell from a stem cell—called spermatogenesis—takes approximately 70 to 90 days. This means the sperm you ejaculate today began its journey about three months ago. The lifestyle choices you make right now will directly impact the sperm that are maturing for release in the next season.
This is actually great news. It gives you a clear timeline. Commit to changes today, and you can expect to see measurable improvements in a semen analysis in about three months. It’s a project with a deadline, and you are the project manager.
Section 1: The Lifestyle Levers – What to Stop & Start
1. Thermal Regulation: Keep the Balls Cool
Your testes hang outside your body for a critical reason: they need to be about 2-4°C cooler than your core temperature to produce healthy sperm.
- The Risks: Chronic heat exposure is a silent saboteur. This includes:
- Tight Clothing: Swap tight briefs for loose-fitting boxers. The data on this is mixed, but if you have borderline parameters, it’s a zero-cost experiment.
- Prolonged Heat: Long, hot baths, frequent sauna or hot tub sessions (more than 30 minutes, multiple times a week).
- Laptops on Laps: The combination of device heat and closed-leg posture raises scrotal temperature.
- Heated Car Seats: Long commutes on high heat.
- The Fix: Think airflow and moderation. Choose loose pants, limit hot tub time, put a pillow under your laptop, and turn down the heated seat.
2. Tobacco, Cannabis, & Recreational Drugs: Just Stop.
The data is unequivocal here.
- Smoking: Tobacco smoke contains thousands of toxins that increase oxidative stress, directly damaging sperm count, motility, morphology, and DNA. It’s one of the worst things you can do for fertility.
- Cannabis: Regular use can lower sperm count and suppress the hormones that drive sperm production. It can also affect libido and erectile function.
- Anabolic Steroids & Other Drugs: Shut down your body’s natural testosterone production, collapsing sperm count to zero. The effects can be long-lasting or permanent.
3. Alcohol: It’s About Dose and Frequency.
- Heavy/Regular Use: Defined as more than 15-20 drinks per week, is linked to lower testosterone, reduced sperm production, and increased abnormal forms.
- Moderate/Occasional Use: (e.g., a few drinks per week) likely has a minimal impact for most men. However, if you’re already facing challenges, cutting back or taking a 90-day break is a prudent step.
4. Exercise & Body Composition: Find the Sweet Spot.
Fertility follows a U-shaped curve with exercise.
- The Sedentary Side (Obesity): Excess body fat, especially abdominal fat, leads to higher estrogen levels and increased scrotal temperature, harming sperm parameters. It’s also linked to hormonal imbalances.
- The Overtraining Side: Extreme endurance exercise (like marathon or ultra-marathon training) can create systemic inflammation and oxidative stress that temporarily lowers sperm quality.
- The Sweet Spot: Regular, moderate exercise. Aim for 30-60 minutes of brisk activity most days. Strength training is also excellent for boosting testosterone naturally. The goal is a healthy BMI and a sustainable fitness routine.
Section 2: The Dietary Foundation – Fueling Spermatogenesis
Forget magic pills. Think of food as the raw material for building elite sperm. Here are the key nutrients:
- Antioxidants: Your sperm are vulnerable to attack by unstable molecules called free radicals (oxidative stress). Antioxidants are the defense team.
- Vitamin C & E: Found in citrus fruits, berries, nuts, seeds, and leafy greens.
- Selenium & Zinc: Crucial for sperm structure and testosterone production. Find them in Brazil nuts (just 2-3 a day!), shellfish, pumpkin seeds, and lean red meat.
- Omega-3 Fatty Acids: These are the building blocks of the sperm cell’s fluid membrane, essential for motility and the ability to fuse with an egg. Sources: Fatty fish (salmon, mackerel, sardines), walnuts, flaxseeds, chia seeds.
- Folate: Not just for women. Folate is vital for DNA synthesis and repair. Low folate in men is linked to higher sperm DNA fragmentation. Load up on leafy greens, lentils, and avocados.
Your Sperm-Healthy Plate: Fill half with colorful vegetables and fruits (antioxidants), a quarter with lean protein or fatty fish (omega-3s, zinc), and a quarter with whole grains. Sprinkle with nuts and seeds.

What About Supplements?
A high-quality multivitamin can cover basic gaps. For targeted support, supplements like Coenzyme Q10 (CoQ10) have good evidence for improving sperm count and motility by boosting cellular energy. Think of supplements as reinforcing a good diet, not replacing it. Always discuss with your doctor.
Section 3: Environmental & Occupational Factors (The Hidden Influences)
We live in a sea of low-level chemicals that can act as endocrine disruptors, mimicking or blocking hormones.
- Where They Lurk: Certain plastics (BPA, phthalates), pesticides on non-organic produce, parabens in personal care products, and heavy metals.
- Practical Reduction Tips:
- Plastics: Never microwave food in plastic containers. Swap plastic water bottles and food storage for glass or stainless steel.
- Produce: Wash all fruits and vegetables thoroughly. Consider buying organic for the “Dirty Dozen” (e.g., strawberries, spinach, kale).
- Personal Care: Read labels. Opt for phthalate- and paraben-free shampoos, soaps, and lotions.
- Occupational Hazards: Exposure to lead, industrial solvents, pesticides, and prolonged radiation (e.g., welders) can impact fertility. If you work with these, use all recommended protective equipment and discuss concerns with an occupational health specialist.
Section 4: Medical Factors & When to Get Tested
Lifestyle is powerful, but some issues require medical insight.
- Common Medical Conditions:
- Varicocele: A varicose vein in the scrotum that raises local temperature. It’s the most common correctable cause of male infertility.
- Hormonal Imbalances: Low testosterone, high prolactin, or thyroid issues.
- Past Infections: Mumps after puberty, or sexually transmitted infections that caused scarring.
- History of Undescended Testicles.
- Certain Medications: Testosterone replacement therapy, some blood pressure meds, antidepressants.
- The Semen Analysis: Demystified.
This is the essential first test. It’s non-invasive, and provides the data you need. You’ll provide a sample (usually via masturbation) at a lab or clinic after 2-5 days of abstinence. The results give you and your doctor the baseline to work from. - When to Get Tested: Don’t wait for years. The general guideline:
- If you and your partner are under 35, try for 12 months first.
- If she is 35 or older, get a semen analysis after 6 months of trying.
- Get one immediately if there are known risk factors: a history of testicular problems, chemotherapy, or if your partner has known fertility issues.
Section 5: The Partner’s Role: A Team Approach
For the partner reading this: your support is invaluable, but the approach matters.
- Frame it as a “Health Project,” Not a Fix: Say, “Let’s both get as healthy as we can for this,” rather than, “You need to fix your sperm.”
- Cook Together: Make the male fertility diet plan a couple’s adventure. Try new salmon recipes, make big salads.
- Join the Changes: If you’re both cutting back on alcohol or prioritizing sleep, it feels like shared commitment, not a solo burden.
- Provide Emotional Support: The pressure to perform on schedule can be intense. Reassure him that his worth is not tied to a semen analysis result. Reduce pressure around timed intercourse when possible.
Conclusion: An Investment in Your Future
Optimizing your sperm health is not a punishment or an admission of failure. It is one of the most direct investments you can make in your own health, your future child’s health, and your shared dream of a family.
You have the timeline (90 days), the knowledge (lifestyle, diet, environment), and the power to act. Start today. Make one change—swap the underwear, add a handful of walnuts, skip the second beer. In three months, you’ll have a new army of sperm, forged by your better choices, ready for the most important mission of their existence.
Frequently Asked Questions (FAQ)
Do laptops/wifi really damage sperm?
The primary risk from laptops is heat, not WiFi radiation. Placing a laptop directly on your lap for extended periods significantly raises scrotal temperature. Use a desk or a lap desk. The evidence on cell phone radiofrequency waves is mixed and inconclusive, but keeping your phone out of your front pocket is a simple, precautionary step.
How long should I abstain before trying to conceive or a semen analysis?
The “sweet spot” is 2-5 days of abstinence. Shorter abstinence (less than 2 days) may lower count; longer abstinence (over 5-7 days) can increase the number of old, less motile sperm and DNA fragmentation. For timed intercourse, every other day during the fertile window is perfect.
Can cycling hurt fertility?
Prolonged, intense cycling (especially on a hard, narrow seat) can compress nerves and blood vessels, potentially causing numbness and affecting erectile function. It may also increase scrotal temperature. If you’re a serious cyclist and have concerns, consider a ergonomic seat, padded shorts, taking breaks, and getting a baseline semen analysis.
My job is stressful—is that a major factor?
Chronic, severe stress can elevate cortisol levels, which may indirectly suppress testosterone and sperm production. However, everyday work stress is unlikely to be a primary cause of infertility. The negative impact of worrying about fertility stress is often greater. Focus on proven lifestyle factors first, and manage stress through exercise, sleep, and hobbies for your overall well-being.
What’s the deal with soy and testosterone?
This is a pervasive myth. The phytoestrogens in soy are weak and behave differently than human estrogen. Numerous studies show that moderate soy consumption (1-2 servings daily) has no meaningful effect on testosterone or estrogen levels in men. Don’t avoid tofu or edamame based on this misinformation.

