Introduction: From Guesswork to Knowledge
You’ve decided you’re ready to try for a baby. You know timing is everything, but your cycle feels like a mysterious, moving target. An app gives you a predicted ovulation day, but what if it’s wrong? A friend swears by a certain test, but you get a confusing, faint line. You’re left feeling like you’re trying to hit a bullseye in the dark.

This feeling is so common, and it’s exactly why learning to track your own ovulation is a game-changer. It transforms family planning from a game of chance into an act of empowered knowledge. Whether you’re hoping to conceive, aiming to avoid pregnancy naturally, or simply want to understand your body’s rhythms, precise tracking is your key.
As a fertility awareness educator for over a decade, I’ve guided thousands of people from confusion to clarity. This guide is your comprehensive map. We’ll move beyond vague predictions and explore the tangible, biological signs your body gives you each cycle. We’ll break down every major method, from free and simple to tech-enhanced, so you can choose the ovulation tracking methods that fit your life and give you the confidence you deserve.
Ovulation 101: What Are We Actually Tracking?
Before we dive into methods, let’s understand the event we’re pinpointing. Ovulation isn’t random; it’s the grand finale of a precise hormonal symphony each cycle.
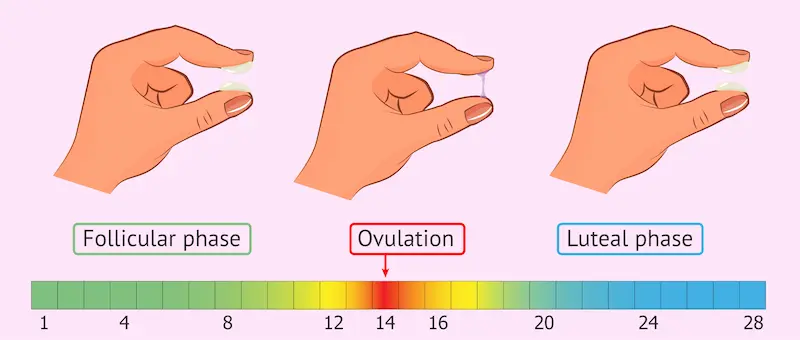
- Follicular Phase: Your cycle begins with your period. Your brain releases Follicle-Stimulating Hormone (FSH), which tells your ovaries to start maturing an egg in a tiny sac called a follicle.
- Estrogen Rises: As the follicle grows, it produces estrogen. Rising estrogen has two key jobs we can track: it changes your cervical mucus (making it fertile and sperm-friendly) and, eventually, it triggers a surge of the next hormone.
- The LH Surge: A spike in Luteinizing Hormone (LH) is the direct trigger for ovulation. This is what ovulation predictor kits detect. Ovulation typically occurs 24-36 hours after the LH surge begins.
- Ovulation: The mature egg is released from the ovary and travels into the fallopian tube. This is the single day of ovulation.
- Progesterone Rises: After the egg is released, the empty follicle becomes the corpus luteum, which pumps out progesterone. This hormone raises your basal body temperature and prepares the uterine lining for a potential pregnancy. This temperature shift is how we confirm ovulation happened.
The goal of tracking is to identify your fertile window—the 5-6 days leading up to and including ovulation. Sperm can live inside you for up to 5 days, but the egg only lasts about 24 hours. By identifying the lead-up, you maximize your chances.
Section 1: The Symptothermal Method – The Gold Standard
This is the most comprehensive approach, combining multiple primary fertility signs. It’s evidence-based, highly effective, and gives you a complete picture.
Cervical Mucus Tracking: Your Body’s Natural Lubricant & Predictor
This is observing the changes in the fluid produced by your cervix. Rising estrogen changes its quantity and quality to support sperm survival and transport.
- How to Track: Check toilet paper or your fingertips throughout the day. Notice sensation (dry, wet, slippery) and appearance.
- The Pattern:
- After Period: Often dry or no noticeable mucus.
- Approaching Ovulation: Mucus appears—first sticky or creamy, then becomes increasingly clear, stretchy, and slippery, resembling raw egg white. This is peak fertile mucus.
- After Ovulation: Under progesterone’s influence, mucus quickly dries up or becomes thick and sticky again.
- Its Role: A predictor of fertility. The presence of egg-white mucus means you are in your fertile window and ovulation is likely approaching.
Basal Body Temperature (BBT) Tracking: The Confirmation
BBT is your body’s temperature at complete rest. The rise in progesterone after ovulation causes a slight but sustained increase in this resting temperature.
- How to Track: Use a sensitive digital BBT thermometer (with two decimal places). Take your temperature immediately upon waking, before you sit up, talk, or drink water—ideally at the same time each morning.
- The Pattern: You’ll see lower temperatures in the follicular phase. After ovulation, you’ll see a clear shift (typically 0.4 to 1.0 degrees Fahrenheit) that stays elevated until your next period. This creates a biphasic pattern on your chart.
- Its Role: A confirmation that ovulation has already occurred. It does not predict ovulation in advance. This is crucial for how to confirm ovulation happened.
Together: Tracking mucus tells you when to try; the temperature shift confirms you’ve ovulated and can stop. This synergy is powerful.
Cervical Position (Optional):
Your cervix itself changes. During the fertile window, it becomes high, soft, and open (like your lips). After ovulation, it becomes low, firm, and closed (like the tip of your nose). This takes practice to discern.
Section 2: Ovulation Predictor Kits (OPKs) & Digital Monitors
These are the most popular tools for those actively trying to conceive. They detect the LH surge in your urine.
- How They Work: They are similar to pregnancy tests. A control line always appears. When the test line is as dark as or darker than the control line, you have a positive result, indicating your LH surge has begun.
- Types:
- Test Strips: Inexpensive, sold in bulk. Great for frequent testing.
- Digital Readers: More expensive, but provide a clear “yes/no” or smiley face reading, removing line ambiguity.
- Crucial How-To Advice for the Best Time to Take an Ovulation Test:
- Start Time: Don’t start too early. Begin testing around cycle day 10-12 for a typical 28-day cycle. If cycles are longer, start later.
- Time of Day: LH is synthesized in the morning but may not appear in urine until afternoon. Test between 10 am and 8 pm. Avoid first-morning urine. Many find 2 pm ideal.
- Consistency: Test at the same time each day and limit fluids for 2 hours before to avoid diluting your urine.
- The Limitation: A positive OPK means ovulation is likely coming soon. It does not guarantee an egg will be released (this can happen in anovulatory cycles). It also doesn’t tell you if ovulation actually occurred. Combining with BBT is a powerful way to confirm.
Section 3: Technology & Apps: From Basic Logs to Wearable Sensors
Cycle Tracking Apps
Think of apps like Flo, Clue, or Kindara as intelligent data diaries. They are only as good as the data you put in.
- Predictive-Only Apps: If you only input your period start date, they use population averages to guess your ovulation. This is often inaccurate.
- Symptothermal/BBT Apps: When you input daily BBT and mucus data, the app’s algorithm can help you identify your shift and confirm ovulation based on your unique signs.
Wearable Technology & Advanced Monitors
This is the high-tech frontier of fertility monitoring wearable devices.
- Temping Wearables (e.g., Tempdrop, Ava): You wear a sensor on your arm or wrist at night. It automatically tracks your resting temperature and other physiological parameters, syncing data to an app. This solves the problem of inconsistent wake-up times and makes BBT charting for beginners much easier.
- Hormone Monitors (e.g., Mira, Inito): These are handheld devices that analyze actual hormone concentrations (LH and estrogen) in your urine using test wands and a digital reader. They provide numerical hormone levels, helping you see your personal baseline and precise surge, which is especially helpful for those with tracking ovulation with irregular periods.
Pros: Convenience, automation, precise data. Cons: Significant upfront cost.
Section 4: Choosing Your Method(s): A Decision Guide
There’s no single “best” method—only the best one for you. Use this guide to match your personality and goals.
- For the Data-Lover / Detail-Oriented (The Detective):
- Method: The full Symptothermal Method (BBT + Cervical Mucus + optional cervix).
- Why: You want the most complete, self-confirming picture. You don’t mind a daily routine and enjoy interpreting your own chart. This provides the highest level of body literacy.
- For Those Actively Trying to Conceive & Want a Clear Signal (The Goal-Oriented):
- Method: Ovulation predictor kits (strips or digital), ideally combined with BBT tracking for confirmation.
- Why: OPKs give a clear, advance “go” signal for timed intercourse. Adding BBT confirms the process was successful, provides data on your luteal phase length, and prevents you from missing a surge if you test at the wrong time.
- For Tech Enthusiasts / Those Who Value Convenience (The Modernist):
- Method: A wearable temperature sensor or a multi-hormone monitor.
- Why: You want accurate data without the daily hassle of manual temping or interpreting test strips. The cost is worth the convenience and high-tech insight.
- For General Awareness & Cycle Regulation (The Observer):
- Method: Basic app logging + paying attention to cervical mucus ovulation signs.
- Why: You want to understand your cycle patterns, predict your period, and get a general sense of your fertile time without intense daily tracking.

Section 5: Putting It All Together – Your Action Plan
Step 1: Pick One Primary Method to Start. Don’t overwhelm yourself. If you’re new, start with observing cervical mucus for one cycle, or try OPKs.
Step 2: Gather Your Tools. A BBT thermometer, OPK strips, or a dedicated notebook/app.
Step 3: Commit to One Full Cycle. Track daily. For BBT, be as consistent as possible. For mucus, check multiple times a day.
Step 4: Record Faithfully. Input data into your app or chart every day.
Step 5: Review at Cycle’s End. Did you see a pattern? A mucus peak? A temperature shift? A positive OPK?
Step 6: Refine. Next cycle, you’ll know when to start OPK testing or what to look for in your mucus. Patterns become clearer over 2-3 cycles.
Common Pitfalls & Fixes:
- Inconsistent BBT Time: Use a wearable or set a very regular sleep schedule.
- Misreading Mucus: Look for the most fertile sign of the day. The sensation of slipperiness is a key clue.
- Starting OPKs Too Late: If you get a positive immediately, you may have missed the start of your surge. Start testing earlier next cycle.
- Conflicting Signals: If your OPK is positive but you see no fertile mucus, trust the OPK for timing intercourse, but note the discrepancy. Your body may be having an anovulatory surge.
Conclusion: Your Body, Your Knowledge, Your Power
Learning how to track your ovulation is more than a means to an end. It is a profound journey into body literacy. It’s the process of learning a unique language—the language of your own hormones and cycles.
This knowledge is a lifelong superpower. It demystifies your health, informs conversations with your doctor, and places the power of understanding squarely in your hands. Whether your goal is a baby, natural birth control, or simply self-awareness, move forward with the confidence that comes from no longer guessing, but truly knowing.
Frequently Asked Questions (FAQ)
How long after a positive OPK do you ovulate?
Ovulation typically occurs 24-36 hours after the onset of the LH surge. Since a positive OPK detects the surge already in progress, ovulation usually happens within 12-36 hours of your first positive test.
Can you ovulate without a temperature shift?
A sustained temperature shift is the primary sign that progesterone has risen, which only happens after ovulation. While occasional anovulatory cycles can have small fluctuations, a true ovulation should be followed by a clear, sustained thermal shift. If you consistently see fertile mucus and positive OPKs but no shift, it may indicate a luteal phase defect or anovulation, warranting a doctor’s visit.
Do I need to track if my cycles are regular?
Regular cycles suggest regular ovulation, but they don’t confirm its exact timing. You could have a 28-day cycle but ovulate on day 14 one month and day 18 the next. Tracking tells you what’s actually happening in the current cycle.
What if I never see ‘egg white’ cervical mucus?
Some people don’t produce abundant mucus. You may only notice a sensation of wetness or see creamy mucus, which is still fertile. Staying well-hydrated can help. If you see no fertile-quality mucus at all, it’s worth mentioning to a healthcare provider, as it can be associated with certain conditions.
How do I track if I have irregular cycles or PCOS?
Irregular cycles make predictive apps useless and can make OPK testing frustrating (you might test for many days or have multiple surges). The most reliable approach is to combine methods. Tracking ovulation with irregular periods often works best with: 1) Daily cervical mucus observation to catch any fertile patches, and 2) Using a wearable BBT sensor to confirm ovulation whenever it happens, without the guesswork of when to start temping. Hormone monitors that track estrogen can also help predict a true LH surge amidst possible false ones common in PCOS. Consulting a reproductive endocrinologist is highly recommended.

