Introduction: The Body That Built a Person
Let’s start with a moment you might recognize. It’s your six-week postpartum checkup. You’re asked, “How are you doing?” You muster a smile. “Fine,” you say. But inside, you’re thinking about the leak when you sneezed yesterday. The strange, heavy feeling in your pelvis when you stand too long. The way your core feels like a hollowed-out bowl. You’re handed a vague instruction: “Do your Kegels.” You try, but you’re not even sure you’re doing them right. The silent question hangs: Is this just how my body is now?
I want you to hear this clearly: No, this is not your new normal. What you are experiencing is common, but it is not inevitable. The narrative that Kegels are the singular answer to postpartum pelvic floor recovery exercises is not just incomplete—it can be counterproductive. Recovery isn’t about clenching in isolation; it’s about re-educating a system that has been through an extraordinary event. It’s about connection, coordination, and compassionate rebuilding.
For a decade in my physical therapy practice, I’ve guided thousands of women through this exact journey. The path to feeling strong, confident, and capable in your postpartum body doesn’t start with a hard contraction. It starts with breath, awareness, and understanding when to seek a guide. This article is that first step. We’ll move beyond Kegels postpartum, explore a safe, phased exercise approach, and, most importantly, outline the undeniable signs that tell you it’s time to seek the hands-on expertise of a specialist.
What Is the Pelvic Floor, and What Did Birth Do to It?
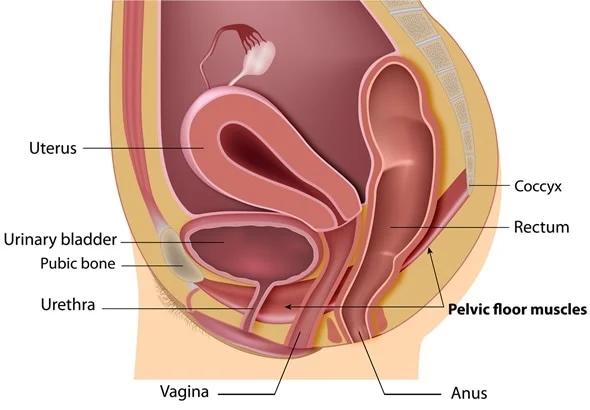
Imagine your pelvic floor not as a single muscle, but as a sophisticated, woven hammock or a bowl. This dynamic group of muscles and connective tissue stretches from your pubic bone in the front to your tailbone in the back, and between your sitting bones. Its job is monumental: it supports your bladder, uterus, and rectum like a trampoline, provides sphincter control for your urethra and anus, plays a key role in sexual function, and works in harmony with your deep abdominals and diaphragm to stabilize your core and spine.
Now, consider what it endured. For nine months, it supported the increasing weight of your growing baby and uterus—like a trampoline with a ever-heavier bowling ball on it. During birth, whether vaginal or surgical, these tissues were stretched, compressed, and potentially scarred. A vaginal delivery can involve profound stretching, potential tearing, and nerve compression. A c-section spares the pelvic floor from descent but involves cutting through the abdominal and uterine walls, severing nerves, and creating a significant demand on the core for protection and healing afterward.
The result? This brilliant system can be left in a state of weakness (unable to support or contract well), or tightness (guarding and unable to relax), or—very often—a confusing combination of both. This is why a one-size-fits-all “just do Kegels” approach fails so many.
The Critical Insight: Beyond Weakness, Understanding a Tight Pelvic Floor
Here is the paradigm shift I see daily in my clinic: more postpartum women are struggling with a pelvic floor that is too tight and non-relaxing than one that is purely weak. Think about it. After trauma (and birth is physical trauma), muscles often guard. They clench to protect. This can lead to a hypertonic pelvic floor—muscles that are chronically tense.
The symptoms of a tight pelvic floor can mimic weakness: leaking urine after baby exercises like jumping, a feeling of urgency, and even the sensation of heaviness. But if you pile Kegels on top of an already clenched muscle, you’re adding tension to tension. This can worsen pain, contribute to painful intercourse postpartum, and prevent true healing. Recovery, therefore, must always begin with the ability to release and relax these muscles, not just contract them.
The Foundational First Step: Diaphragmatic Breathing & The Mind-Muscle Connection
Before you even think about a Kegel, we start here. This is the non-negotiable foundation of all postpartum core restoration.
- Find a comfortable position on your back with knees bent, or propped up on pillows.
- Place one hand on your chest and one on your lower belly.
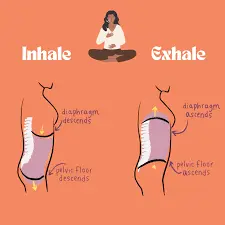
- Inhale slowly and deeply through your nose, directing the breath down into your ribs and belly. Feel your lower hand rise. As you do this, imagine your pelvic floor “hammock” gently widening and descending—a soft, letting-go sensation.
- Exhale slowly through your mouth, letting your belly fall naturally. As you exhale, think of a gentle, upward lift of the pelvic floor—like a light elevator rising one floor. Not a hard squeeze, just a gentle engagement.
- Repeat for 5-10 breaths, focusing on the wave-like motion: Inhale to expand and soften, exhale to gently engage and lift.
This practice re-establishes the neurological connection you may feel you’ve lost (“Where are they?”). It’s your first and most important exercise. Do this multiple times a day.
Section 1: The Progressive Exercise Guide (Weeks 0-6 and Beyond)
Phase 1: The Initial Weeks – Rest & Reconnection (0-6 weeks)
The goal here is healing, not fitness. Always follow your OB/GYN or midwife’s clearance.
- Continued Breathwork: As described above.
- Gentle Pelvic Tilts: Lying on your back with knees bent, inhale to relax. Exhale, gently rock your pubic bone upward, flattening your lower back slightly into the floor. Inhale to release. This gently engages deep abdominals.
- Ankle Glides/Heel Slides: Lying on your back, slowly slide one heel along the bed to bend your knee, then slide it back. Alternate. Focus on keeping your core and pelvis stable.
- Short, Gentle Walks: Start with 5-10 minutes, focusing on good posture. This promotes circulation and healing.
Phase 2: Rebuilding Foundations (~6 weeks+, with clearance)
Now we integrate gentle strength with your newfound connection.
- Functional Kegels: Using your breath connection, practice a gentle pelvic floor lift on the exhale. Hold for 2-3 seconds, then release fully on the inhale for twice as long. Aim for 5-10 reps, 2-3 times a day. Quality over quantity.
- Gentle Bridges: Lying on your back with knees bent. Inhale to prepare. Exhale, engage your pelvic floor and glutes, and lift your hips toward the ceiling until your body forms a straight line from knees to shoulders. Inhale at the top, exhale to lower slowly. This teaches glute and pelvic floor coordination.
- Seated Marching: Sit tall on a stable chair. Engage your core and lift one foot an inch off the floor, hold for a moment, lower, and alternate. This builds stability in a functional seated position.
Phase 3: Integrating Strength (~12 weeks+, with continued comfort)
Focus on core coordination over isolated strength.
- Mini-Squats: Stand with feet hip-width. Inhale, send hips back as if sitting in a chair. Exhale, engage pelvic floor and core, return to stand. Ensure knees track over toes.
- Bird-Dog: On hands and knees. Inhale to prepare. Exhale, engage core, and slowly extend opposite arm and leg, keeping your spine and pelvis stable. This challenges coordination and global stability.
- Modified Plank (Forearm or Elevated): Start with hands on a sturdy table or couch. Maintain a straight line from head to heels, engaging your deep core to prevent sagging or arching. Start with 10-15 second holds.
- Standing Marches: Like seated marching, but standing, focusing on maintaining a stable, tall pelvis with each leg lift.
Section 2: The Red Flags When to See a Pelvic Floor Physical Therapist
While the above guide is a safe starting point, these symptoms are your body’s clear signal that you need a personalized assessment. Seeking pelvic floor therapy after birth is a proactive, intelligent step, not a last resort.
Consult a pelvic floor PT if you experience:
- Persistent Leakage: Any urinary or fecal leakage that continues beyond the first few weeks, or that appears with coughing, sneezing, jumping, or running.
- Sensation of Heaviness, Pressure, or Bulging: A feeling that something is falling out of your vagina, especially after standing all day or with bowel movements. These are potential signs of prolapse after childbirth.
- Pain with Intercourse (Dyspareunia): Pain that persists beyond 8-12 weeks postpartum, when tissues should have healed. This is often related to pelvic floor muscle tension or scarring.
- Persistent Pain: Ongoing pain in your lower back, hips, tailbone (coccyx), or pelvis that doesn’t resolve with rest.
- Concerning Diastasis Recti: A gap in your abdominal muscles that feels very deep, doesn’t improve with gentle postpartum diastasis recti exercises safe like breathwork and pelvic tilts, or causes a visible doming or bulging during activity.
- No Mind-Muscle Connection: A complete inability to feel or control your pelvic floor muscles, despite focused practice.
- Pain with Kegels or Bearing Down: If contracting your pelvic floor or straining for a bowel movement causes pain, this indicates dysfunction that needs assessment.
Section 3: What to Expect in Pelvic PT (Demystifying the Process)
The thought of an internal exam can be intimidating. Let me demystify it. A pelvic floor physical therapist is a specialist who treats this area with the same clinical professionalism as a knee or shoulder.
- Comprehensive Interview: We’ll discuss your birth story, symptoms, and goals.
- External Exam: We assess your posture, core, hip, and spinal mobility, and check for diastasis recti.
- Internal Exam (Vaginal and/or Rectal): This is always explained, consensual, and clinical. We use a single gloved finger to assess muscle tone, strength, coordination, and tenderness from the inside, where these muscles live. It’s the only way to accurately diagnose if muscles are weak, tight, or uncoordinated. It should not be painful.
- Personalized Plan: Based on the findings, you’ll get a customized home program, which may include manual therapy (internal or external to release tight tissues), biofeedback (using sensors to help you “see” your muscle activity), and specific exercise progressions.
The Big Picture: Integrating Protection into Motherhood
Recovery happens between exercise sessions. Protect your healing pelvic floor by:
- Lifting Smart: Exhale and engage your core before lifting your car seat, toddler, or groceries. Hold the load close to your body.
- Log Rolling Out of Bed: Roll onto your side, use your arms to push up to a seated position, rather than doing a painful “sit-up” to get out of bed.
- Managing Constipation: Drink plenty of water, eat fiber, and use a small footstool (“Squatty Potty”) to avoid straining.
Conclusion: Your Strength is in Your Story
Your postpartum body is not broken. It is a testament to resilience. The journey of postpartum pelvic floor recovery is not about returning to a former version of yourself, but about rebuilding a foundation of strength and confidence for the mother you are now.
Listen to your body’s signals—both the ones that say “I’m ready to try a little more” and the clear red flags that say “I need a guide.” Seeking help is not a failure; it is the ultimate act of advocacy for your own well-being. You built a person. Now, with knowledge, patience, and the right support, you can rebuild the strong, capable core that will carry you through motherhood.
Frequently Asked Questions (FAQ)
Is it too late if I’m 1/2/5 years postpartum?
It is never too late. The pelvic floor muscles are responsive to training at any stage. Many women seek and find tremendous help years after their last child. Your body can still heal and strengthen.
Can I do these exercises after a c-section?
Absolutely, and it’s crucial. While the pelvic floor didn’t go through a vaginal delivery, pregnancy alone loaded it for nine months, and a c-section is major abdominal surgery. The phased approach, starting with breathwork and gentle connection, is perfect. Pay close attention to your incision site and avoid any exercise that causes pulling or pain there.
What if I can’t feel my pelvic floor at all?
This is extremely common and called “pelvic floor amnesia.” This is a primary reason to see a pelvic floor PT. We use techniques like biofeedback and precise manual cues to help you “find” those muscles again. The breathwork described is your first and best home tool.
Are squats safe for the pelvic floor?
Yes, when performed with good form and proper core engagement. The mini-squat in Phase 3 is a safe start. The key is to exhale and engage your pelvic floor/core as you stand up, which supports the pelvic floor against downward pressure. Avoid going too deep or adding weight until you have mastered the coordination pain-free.
How do I know if my diastasis recti is improving?
You can perform a gentle self-check: Lie on your back with knees bent. Place your fingers horizontally just above your belly button. Lift your head and shoulders slightly off the floor. Feel for a gap, the depth of the gap (can you sink your fingers in?), and the tension of the tissue under your fingers. Improvement is marked not just by a narrowing gap, but by a feeling of firm tension rising under your fingers as you lift your head. If you see doming or “coning” of your abdomen during daily movements or exercise, you need to regress to simpler exercises like breathwork.

