Introduction: More Than Just Dry Skin
If you’re reading this, I imagine you’ve spent countless nights watching your baby struggle against that relentless itch. You’ve probably tried every cream on the shelf, only to see those red, rough patches return with a vengeance. That feeling of helplessness when your infant cries, rubbing their tender cheeks against your shoulder—it’s profoundly draining. Many parents in my clinic express this same frustration, coupled with a nagging worry: “Is this just skin deep, or is something else going on?”

Let me reassure you first: your concern is not only valid but crucial. That persistent infant eczema might be your baby’s first visible sign of a broader conversation their immune system is trying to have. What we’ve learned over the past decade is revolutionary—the skin is not just a passive barrier. In babies with eczema, it’s an active player in a complex drama that can involve the immune system and, yes, reactions to foods.
Consider Leo, a five-month-old I saw recently. His mother, Sarah, was exclusively breastfeeding and meticulous about her baby’s care. Yet, Leo developed severe eczema on his cheeks and the bends of his elbows. Sarah had cut out dairy on a friend’s suggestion, saw slight improvement, but was left confused, exhausted, and worried about her own nutrition. Her story is incredibly common, and it sits right at the intersection of infant skin health and maternal diet.
This guide aims to walk you through this intricate landscape. We’ll explore the genuine connection between baby eczema and food allergies, equip you with a solid, multi-pronged baby eczema management routine, and provide a thoughtful, evidence-based roadmap for any breastfeeding mom considering an elimination diet. My goal is to replace your anxiety with understanding and your confusion with a clear, actionable plan.
What Infant Eczema Really Looks Like: Beyond Simple Dryness
Many newborns have peeling skin or occasional dry patches. So, how can you tell if it’s truly atopic dermatitis, the medical term for eczema? It’s about the pattern, persistence, and presentation.
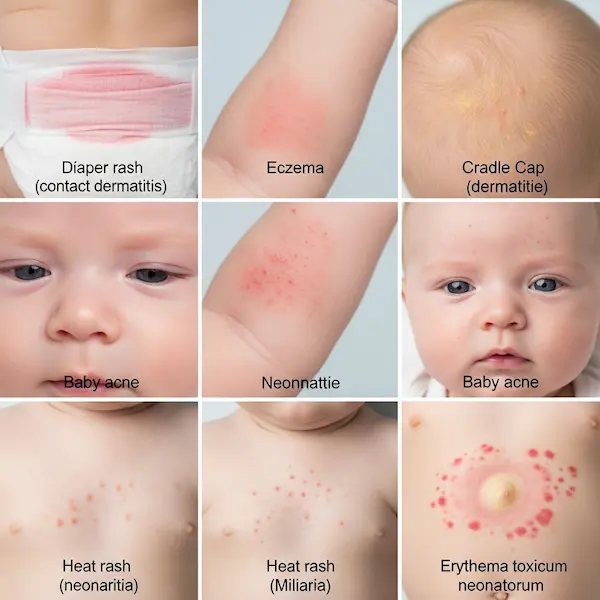
Classic infant eczema often starts between 2 and 6 months of age. It frequently appears first on the cheeks and scalp as red, scaly, sometimes oozing patches. Unlike transient dryness, it’s intensely itchy—you might notice your baby rubbing against sheets or your clothes before they can even scratch. As they grow, the rash often moves to the extensor surfaces (the outsides of elbows and knees), and later, in toddlers, to the flexural areas (the insides of elbows and knees).
The skin isn’t just dry; it’s inflamed. You might see tiny red bumps, rough leathery patches (lichenification) from chronic rubbing, and in lighter skin tones, a pronounced redness. In darker skin tones, eczema can appear ashen brown, purple, or grey, and may be more focused on follicular bumps. Persistent scratching can lead to broken skin, bleeding, and sadly, secondary bacterial infections, which show up as honey-colored crusts, pustules, or increased warmth and swelling.
[Image Suggestion URL: A side-by-side comparison collage showing common infant dry skin versus mild, moderate, and severe infant eczema on different skin tones. Alt text: Visual guide to identifying infant eczema versus common dry skin in babies.]
Recognizing this distinction is the first step in how to identify food triggers for baby eczema. If the rash is simply dry skin, it will likely respond beautifully to consistent moisturizing alone. True eczema, however, often needs more—it’s a clue that the skin barrier is fundamentally compromised.
The Science of the Connection: The “Leaky” Barrier and the Atopic March
To understand the infant eczema food allergy connection, we need to talk about two key concepts: the skin barrier and the atopic march.
Imagine your baby’s healthy skin like a well-built brick wall. The skin cells (keratinocytes) are the bricks, and lipids (fats) are the mortar holding them tightly together. This wall keeps moisture in and irritants, allergens, and microbes out. In babies prone to eczema, due largely to genetic factors, this wall is faulty. The mortar is deficient—it’s “leaky.”
Now, picture that leaky skin wall in your infant’s early months. Everyday substances—dust, pet dander, laundry detergent residues, and yes, food proteins from saliva or spilled milk—can penetrate deeper into the skin than they should. When they do, they encounter immune sentinel cells called Langerhans cells. These cells essentially sound the alarm, telling the immune system, “We have an invader!” This can initiate a localized inflammatory response (the eczema rash) and start sensitizing the systemic immune system to that specific protein.
This is where the atopic march begins. It’s the observed progression where eczema in infancy often precedes the development of food allergies, allergic rhinitis (hay fever), and asthma. The theory is that the damaged, inflamed skin becomes a primary site for allergic sensitization. A baby might first become sensitized to peanut protein, for example, not by eating it, but through tiny particles in household dust contacting their eczematous skin. Later, when they ingest peanut, their already-sensitized immune system reacts more strongly.
It’s a powerful reason why aggressively managing your baby’s eczema is about more than comfort today. It’s a potential strategy for atopic march prevention strategies, aiming to protect that delicate skin barrier to possibly reduce the risk of future allergic conditions.
Common Food Triggers and How Reactions Manifest
When we talk about food-related reactions in the context of eczema, we’re usually discussing two types: IgE-mediated allergies (immediate, can involve hives, vomiting, or anaphylaxis) and non-IgE-mediated sensitivities (delayed, often appearing as worsened eczema or digestive upset). For eczema flares, we’re frequently looking at the delayed, non-IgE type.
The most common culprits, accounting for the vast majority of cases, are:
- Cow’s milk protein
- Egg
- Peanut
- Soy
- Wheat
Reactions aren’t always dramatic. You won’t necessarily see immediate hives or swelling (though if you do, seek medical attention immediately). Instead, think of a slow burn. A breastfeeding mother might have a large glass of milk, and 24-48 hours later, her baby’s cheeks flared a deeper red, the itch seems more intense, or the baby seems fussier and more gassy. It’s this subtle, delayed pattern that makes how to identify food triggers for baby eczema so challenging and why a systematic approach is essential.
It’s also vital to remember that eczema is multifactorial. Food might be one piece of the puzzle, alongside environmental irritants, heat, sweat, stress, and infections. A food trigger won’t cause eczema in a baby without the genetic predisposition, but it can be a significant flare factor in a significant subset of infants.
Your Foundation: A Comprehensive Baby Eczema Management Routine
Before we even consider dietary changes, building a rock-solid daily skincare routine is non-negotiable. This routine aims to repair the “leaky” barrier, reduce inflammation, and break the itch-scratch cycle. Think of this as your baseline; it’s what makes any subsequent dietary investigation possible and meaningful.
1. The Daily Bath and the “Soak and Seal” Method
Contrary to old advice, daily bathing is now recommended. The key is to do it right.
- Bathe Daily: Use lukewarm (not hot) water for 5-10 minutes.
- Use a Gentle Cleanser: Choose a fragrance-free, soap-free, non-foaming cleanser. Use it only on dirty areas (face, neck, hands, diaper area); you don’t need it on the entire body every day.
- Pat Dry, Don’t Rub: Gently pat the skin with a soft towel, leaving it slightly damp.
- The “Seal”: Within 3 minutes of getting out of the bath, apply a generous layer of your prescribed medication (if any) to affected areas. Then, immediately slather the entire body with a thick, eczema safe moisturizer for newborns. We’re talking about ointments (like plain petroleum jelly) or thick creams, not thin lotions. This traps the water from the bath in the skin.
This soak and seal method for infant eczema is the single most effective thing you can do at home. It should be done at least once, ideally twice, a day.
2. Environmental and Laundry Controls
- Dress for Success: Use 100% cotton clothing. Avoid wool and rough synthetics directly against the skin. Keep it loose and cool.
- Laundry: Wash all baby clothes, bedding, and even your own clothes that the baby touches with a hypoallergenic laundry detergent for baby clothes. Avoid fabric softeners and dryer sheets, as residues can be irritating.
- Climate: Keep the home cool and use a humidifier in dry months. Overheating is a major itch trigger.
3. Nail Care and Scratch Prevention
Keep those tiny nails filed short and smooth. Consider using soft cotton mittens or “scratch sleeves” at night to prevent damage from unconscious scratching.
This consistent, gentle care reduces the overall inflammatory load on your baby’s skin. When the skin is calmer and less “leaky,” you get a clearer signal if food is still a contributing factor.
The Breastfeeding Mother’s Guide to Elimination Diets
This is the section many of you are here for. Let’s be clear: an elimination diet is not a first step. It’s a considered step for when optimal skincare hasn’t controlled moderate to severe eczema, or when there are strong clues pointing to food (like a clear history of flare-ups after maternal ingestion of a specific food, or accompanying digestive symptoms in the baby).
Important Disclaimer: This should ideally be done in partnership with your pediatrician, a pediatric allergist, or a registered dietitian. They can confirm the need, help you target the right foods, and ensure nutritional adequacy.
When Should a Breastfeeding Mom Consider an Elimination Diet?
- When your baby’s eczema is moderate to severe and not responding well to consistent topical care and mild topical corticosteroids.
- When there is a clear, reproducible pattern of flare-ups linked to a specific food in your diet.
- When your baby has other symptoms alongside eczema, such as frequent reflux, vomiting, mucous or blood-streaked stools, poor growth, or excessive fussiness.
The Step-by-Step Guide
Step 1: Choose Your Starting Point.
The most common and evidence-based approach is to start with a dairy-free while breastfeeding for baby’s skin trial. Cow’s milk protein is the most frequent offender. You’ll need to eliminate all forms of dairy: milk, cheese, yogurt, butter, and hidden dairy in processed foods (check labels for casein, whey, lactoglobulin). A trial should last a minimum of 2-4 weeks to see if there’s improvement in your baby’s skin.
Step 2: The Food and Symptom Log.
This is your detective’s notebook. Every day, log:
- What you eat and drink.
- Your baby’s skin condition (rate it on a simple scale of 1-5).
- The baby’s itch level, sleep quality, and any digestive symptoms (gas, stool consistency).
- Any potential environmental triggers (hot day, new detergent).
This food and symptom diary for tracking baby eczema triggers is objective gold. Patterns will emerge that guesswork will never reveal.
[Image Suggestion URL: A photo of a simple notebook page with columns for Date, Mom’s Food, Baby’s Skin Score (1-5), Baby’s Sleep, Notes. Alt text: Example of a handwritten food and symptom log for identifying infant eczema triggers.]
Step 3: Reading Labels and Cross-Contamination.
Become a label sleuth. Dairy, egg, soy, and wheat are in countless products. Be aware of cross-contamination if you’re highly sensitive (e.g., “may contain milk” warnings).
Step 4: Maintaining Your Nutrition.
This is critical. Your health directly impacts your milk supply and your ability to care for your baby.
- Calcium: When you cut dairy, you must replace it. Fortified plant milks (almond, oat, soy*), calcium-set tofu, leafy greens (kale, bok choy), and almonds are excellent sources. Consider a calcium supplement (consult your doctor).
- Protein & Calories: Ensure you’re eating enough from other sources like lean meats, poultry, fish, legumes, and whole grains. Don’t undereat.
- Vitamin D & B12: These can be concerns on restricted diets. A prenatal vitamin is often recommended to continue.
Step 5: The Reintroduction Challenge.
If you see significant improvement after 4 weeks, the next step is to confirm the trigger. Under your doctor’s guidance, you would “challenge” by reintroducing the eliminated food. Have a serving of dairy, for example, and monitor your baby closely over the next 24-72 hours for a return of symptoms. If symptoms recur, you have confirmation. If not, that food is likely not a trigger for your baby, and you can move on to investigate another (like egg).
This process requires patience. Eliminating multiple major food groups at once is rarely advised, as it’s overly restrictive, nutritionally risky, and makes identifying the specific culprit impossible.
The Role of Medication: Working with Your Pediatrician
A proactive skincare routine and diet exploration work hand-in-hand with medical treatment, not instead of it. For inflamed eczema, topical corticosteroids (like hydrocortisone 1%) are the first-line anti-inflammatory treatment. Used correctly—a thin layer applied once or twice daily only to red/itchy areas until they clear (usually 3-7 days), then stopped—they are very safe and effective. The fear of “steroids” often leads to under-treatment, prolonging the baby’s discomfort and skin damage.
For persistent areas or as maintenance, your doctor may prescribe a topical calcineurin inhibitor (like pimecrolimus or tacrolimus), which are non-steroid anti-inflammatory creams. These can be used on sensitive areas like the face and for longer-term control.
The goal of medication is to rapidly quell the inflammation so that your diligent skincare and barrier repair efforts can work effectively. It breaks the itch-scratch cycle, prevents infection, and improves sleep for everyone.
A Path Forward, Not Just a Quick Fix
If you take one thing from this guide, let it be this: managing infant eczema linked to food sensitivities is a journey of observation, patience, and consistent care. There is seldom a single “cure,” but there is absolutely a path to excellent control.
You are not just soothing itchy skin; you are actively nurturing your baby’s skin barrier, potentially influencing their long-term immune health, and learning to read their unique bodily signals. The breastfeeding diet for itchy baby is a powerful tool, but it’s one tool in a well-stocked toolbox that includes daily moisturizing, trigger avoidance, and appropriate medical care.
It can feel isolating, but know that you are navigating a very common challenge with newfound knowledge and a solid plan. Trust your instincts, partner with a supportive healthcare team, and celebrate the small victories—a night of better sleep, a smoother patch of skin, a happier, more comfortable baby.
Frequently Asked Questions (FAQ)
Can my baby outgrow this eczema and food allergies?
Many children do see significant improvement or even outgrow eczema as they get older, often by school age. Regarding food allergies, tolerance to milk, egg, soy, and wheat is common (around 50-80% outgrow by age 10). Allergies to peanuts, tree nuts, and seafood are more often lifelong, though not always. Early, effective eczema management and guided early introduction of allergenic foods (as per your pediatrician’s advice) may support positive outcomes.
Is formula feeding better if my baby has eczema?
Absolutely not. Breast milk provides unparalleled immune benefits and is the ideal nutrition. For babies with a confirmed cow’s milk protein allergy who are not breastfed, your pediatrician will recommend a hypoallergenic formula (extensively hydrolyzed or amino acid-based). Switching to a standard formula is not helpful and could worsen symptoms.
Are natural remedies like coconut oil effective?
Pure, virgin coconut oil has antimicrobial properties and can be a good, safe moisturizer for some babies, making it a potential eczema safe moisturizer for newborns. However, it is a moisturizer, not an anti-inflammatory. It’s excellent for the “seal” step but will not calm active, red, inflamed eczema. For that, you need an anti-inflammatory (like a prescribed topical). Always patch-test any new product on a small area first.
What are the signs baby eczema is infected?
Be vigilant for: increased redness, warmth, swelling, yellow or honey-colored crusting, pus-filled bumps, or if your baby develops a fever. Infected eczema (often with staph bacteria) requires prompt medical attention and usually oral antibiotics. Good skincare is the best prevention.
How long does it take to see results from an elimination diet?
For non-IgE mediated reactions (like most eczema flares), it can take 2-4 weeks of strict elimination to see noticeable skin improvement. Gut symptoms may improve faster. This delayed timeline is why meticulous food logging is so important—you need to connect the dots over time.
Remember, you are the expert on your child. Use this information as your map, trust your partnership with your healthcare providers, and know that with careful, loving management, you can calm the storm and give your baby—and yourself—the comfort you deserve.

