Discovering you’re expecting twins is a moment of extraordinary surprise and wonder—followed quickly by a cascade of new questions. A twin pregnancy is a unique journey, classified medically as a “high-risk” pregnancy, but this term speaks to the need for specialized prenatal care for multiples, not to an expectation of problems. It means your body and your babies will be monitored with extra attention to ensure the healthiest outcome for all. This comprehensive guide will walk you through what makes a twin pregnancy different, from the types of twins and increased nutritional needs to the nuanced medical monitoring and essential preparations for bringing two newborns home. Our goal is to replace anxiety with knowledge, empowering you to confidently navigate this remarkable experience.
The First Distinction: Understanding Zygosity and Chorionicity
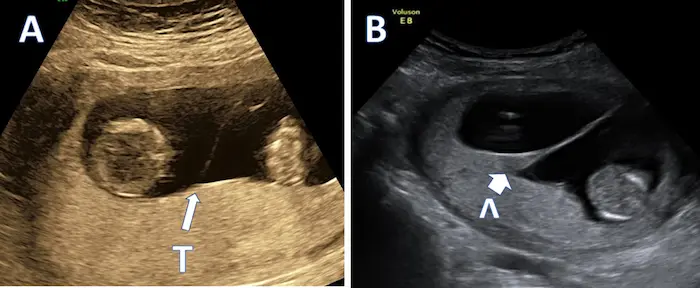
Not all twin pregnancies are the same. The early development of your twins sets the stage for their prenatal care. Your first ultrasound will be crucial in determining this.
- Fraternal Twins (Dizygotic): The most common type, resulting from two separate eggs fertilized by two separate sperm. They each have their own placenta (chorion) and amniotic sac (amnion). This is called a dichorionic-diamniotic (di-di) pregnancy. They are genetically as similar as any siblings and can be same-sex or boy/girl.
- Identical Twins (Monozygotic): Result from a single fertilized egg that splits. The timing of the split determines the type:
- Dichorionic-Diamniotic (Di-Di): The split occurs within the first 3 days. Each twin has its own placenta and sac. This is the lowest-risk identical twin setup.
- Monochorionic-Diamniotic (Mo-Di): The split occurs between days 4-8. Twins share a single placenta but have separate amniotic sacs. This requires closer monitoring for conditions like Twin-to-Twin Transfusion Syndrome (TTTS).
- Monochorionic-Monoamniotic (Mo-Mo): The rarest and highest-risk type, where the split occurs after day 9. Twins share both a single placenta and a single amniotic sac, risking cord entanglement. This requires extremely specialized care and very early delivery.
Why this matters: Your twins’ chorionicity (placenta number) is the most important factor guiding your prenatal care, more so than whether they are identical or fraternal. A di-di pregnancy generally has the lowest risk profile.
The Hallmarks of Twin Prenatal Care: More Frequent Monitoring
From the start, your care will be more intensive, often involving a maternal-fetal medicine (MFM) specialist working alongside your OB-GYN.
- More Frequent Appointments: You’ll see your provider every 2-3 weeks in the second trimester and weekly in the third trimester, compared to the standard schedule for a singleton pregnancy.
- More Ultrasounds: Expect ultrasounds at nearly every visit, especially in a Mo-Di pregnancy. These scans meticulously track each baby’s growth, amniotic fluid levels, and placental health. Growth scans are typically done every 4 weeks, but may be as frequent as every 2 weeks for Mo-Di twins.
- Specialized Screening & Testing:
- The nuchal translucency screening and NIPT (Non-Invasive Prenatal Testing) are both applicable and can screen for chromosomal abnormalities.
- You will be screened early and regularly for gestational diabetes, as the risk is higher with twins.
- Your blood pressure will be closely watched due to the increased risk of pregnancy-induced hypertension and preeclampsia.
Navigating Increased Physical Demands & Symptoms
Carrying two babies means your body is working in overdrive. Symptoms of a singleton pregnancy are often amplified and appear earlier.
- Severe Morning Sickness (Hyperemesis Gravidarum): Higher levels of pregnancy hormones can lead to more intense and prolonged nausea and vomiting.
- Rapid Weight Gain & Earlier Show: You will likely “pop” much sooner. The recommended weight gain for a twin pregnancy is greater (typically 37-54 lbs for a normal BMI) to support healthy fetal growth.
- Pronounced Fatigue: Creating two humans is exhausting. Rest is not a luxury; it’s a medical necessity.
- Intensified Discomfort: Back pain, pelvic girdle pain, heartburn, shortness of breath, and swelling can be more severe and set in earlier due to the increased uterine size and weight.
- Anemia Risk: Your iron needs are substantially higher to support the increased blood volume for two placentas and babies. Iron supplementation is almost always recommended.
Key Risks and Complications to Monitor
Awareness, not fear, is the goal. Your medical team is trained to vigilantly monitor for these conditions.
- Preterm Birth: The single most common “complication.” The average twin pregnancy delivers at 35-36 weeks. A significant goal of care is to safely prolong pregnancy as close to term as possible. You’ll be educated on the signs of preterm labor.
- Preeclampsia: The risk is 2-3 times higher. Monitoring includes regular blood pressure checks and urine tests for protein.
- Gestational Diabetes: The risk is higher due to increased placental mass and hormones that cause insulin resistance.
- Intrauterine Growth Restriction (IUGR) & Discordant Growth: One twin may grow slower than the other. In a shared placenta (Mo-Di) scenario, this can be due to an unequal sharing of resources.
- Twin-to-Twin Transfusion Syndrome (TTTS): A serious complication affecting only Mo-Di twins (shared placenta). Blood vessels in the shared placenta connect the two babies’s circulations unevenly. One twin (the “donor”) gives too much blood to the other (the “recipient”), risking complications for both. Treatment exists, including laser surgery to seal the connecting vessels, which is why frequent monitoring is life-saving.
- Vanishing Twin Syndrome: In very early pregnancy, one twin may miscarry while the other continues to develop. This is often identified on an early ultrasound.
Nutrition & Lifestyle: Fueling a Twin Pregnancy
Your diet is the primary building material for your babies. The caloric increase is modest (about 600 extra calories per day in the later stages), but the need for specific nutrients is critical.
- Protein is Paramount: Aim for at least 100-120 grams of high-quality protein daily (lean meat, poultry, fish, eggs, dairy, legumes, tofu). Protein is essential for building two babies’ tissues and supporting your expanding blood supply.
- Hydration: Drink at least 3 liters of water daily. This helps support increased blood volume, reduces Braxton Hicks contractions, and may help lower the risk of preterm labor.
- Key Supplements: In addition to a high-quality prenatal vitamin, you will likely need additional iron and possibly calcium, magnesium, and vitamin D as directed by your provider.
- Activity & Rest: Moderate exercise like walking, swimming, or prenatal yoga is beneficial, but listen to your body. Your provider may advise scaling back or stopping certain activities earlier than in a singleton pregnancy. Prioritizing rest and reducing stress are non-negotiable components of care.
Preparing for Birth: Setting Realistic Expectations
Planning for a twin delivery requires flexibility. Vaginal birth is possible for many, but the likelihood of a cesarean section (c-section) is higher.
- Vaginal Birth Criteria: Generally considered when:
- Both twins are in a head-down (vertex) position, especially Twin A (the one closest to the cervix).
- You have no other complications (preeclampsia, placenta previa).
- The delivering provider and hospital are experienced in twin deliveries.
- The Role of C-Section: A c-section may be planned or become necessary during labor. It is the recommended route if Twin A is breech, if there’s a significant size difference, if there are signs of fetal distress, or for Mo-Mo twins.
- The Importance of a Level III NICU: It is strongly advised to deliver at a hospital with a Level III Neonatal Intensive Care Unit (NICU), regardless of your birth plan. Twins are more likely to need specialized care after birth, even if born near term.

Postpartum & Newborn Preparation: Thinking in Twos
Practical preparation for two babies requires a different mindset.
- Gear: You don’t need two of everything. Essential duplicates include infant car seats. You will likely need a double stroller. For sleeping, separate bassinets or cribs are recommended for safety.
- Feeding: Whether you plan to breastfeed, formula-feed, or combination-feed, seek guidance. Lactation consultants experienced with twins are invaluable. A twin nursing pillow is a game-changer. Remember, “fed is best,” and feeding two is a logistical feat—give yourself grace.
- Support System: This is the most critical “supply.” Line up help for the postpartum period—family, friends, a postpartum doula. Your recovery will be more demanding, and having hands to help with laundry, meals, and holding one baby while you tend to the other is essential for your mental and physical health.
- Mental Health: The risk of postpartum depression and anxiety is higher after a multiples pregnancy. Be proactive. Discuss a screening plan with your provider and identify your support network.
FAQ: Your Twin Pregnancy Questions, Addressed
Q: Will I definitely deliver early?
A: While early delivery is common, “early” is relative. Many twins deliver in the mid-to-late 30-week range, which is considered “late preterm.” Every day you stay pregnant past 32 weeks is a significant benefit for your babies’ development.
Q: Can I have a natural, drug-free birth with twins?
A: It is possible, but the environment is more medically managed. You will have continuous fetal monitoring for both babies, and an IV line is standard. Discuss your pain management preferences with your provider, but remain open to changes based on the babies’ positions and well-being.
Q: How much bigger will my belly get compared to a singleton pregnancy?
A: Significantly. By the third trimester, you will likely measure full-term for a singleton pregnancy. This contributes to the increased physical discomfort and need for more rest.
Q: Do twins have a higher risk of developmental delays?
A: Prematurity is the primary risk factor for developmental delays, not twinning itself. Twins born at or near term have the same developmental expectations as singletons. Close developmental follow-up is standard for preterm infants.
Q: What’s the most important thing I can do for a healthy twin pregnancy?
A: 1) Attend all your prenatal appointments. Early detection of any issue is key. 2) Prioritize nutrition and hydration. 3) Listen to your body and rest aggressively. 4) Build your support team now.
A twin pregnancy is a journey of extraordinary demands and even more extraordinary rewards. It requires you to be an informed, proactive partner in your care. By understanding the specialized monitoring, respecting your body’s amplified needs, and building a robust plan for birth and beyond, you move from feeling like a high-risk patient to feeling like a capable, prepared parent of multiples. Embrace the unique path. Celebrate each milestone, from seeing two heartbeats on the first ultrasound to finally holding both of your babies in your arms. You are growing a family, and an incredible community of multiple-birth families is ready to welcome you.

