There is a sound that defines pregnancy more than any other—the swift, steady drumbeat of your baby’s heart. That miraculous whoosh-whoosh-whoosh first heard during an early ultrasound becomes the most reassuring rhythm an expectant parent can know. It’s a direct audio line to your baby’s well-being, a biological proof of life thriving in its hidden world.
But beyond the emotional magic, your baby’s heart rate serves a critical medical purpose. It is a vital sign, a window into their neurological development and overall health. This guide will walk you through the entire journey of tracking baby’s heart rate—from when it begins, what’s considered normal, how healthcare providers monitor it, and the important considerations around trying to listen at home. Our goal is to replace anxiety with understanding, helping you interpret this fundamental sign of life throughout your pregnancy and into delivery.
Part 1: The First Heartbeat & Normal Ranges Through Pregnancy
When Does the Heart Begin to Beat?
Your baby’s cardiovascular system is the first organ system to function. Here’s a remarkable timeline:
- Around Week 5: The primitive heart tube begins to form and starts a rhythmic, peristaltic motion. This is not yet the four-chambered heart we know, but it’s the beginning of circulation.
- Week 6-7: The heart tube folds and divides. On a transvaginal ultrasound, you may see the first flicker of cardiac activity, often around 110 beats per minute (BPM).
- By Week 9: The four chambers of the heart are largely formed, and the valves begin to develop. The rate increases rapidly.
What is a Normal Fetal Heart Rate?
One of the most common questions is, “What’s a good heart rate for my baby?” The answer changes as pregnancy progresses.
First Trimester (Weeks 6-13):
- The heart rate starts around 110 BPM at 6 weeks.
- It peaks between weeks 9-10, often reaching 140-170 BPM, sometimes even higher.
- There is a wide range of normal during this period of rapid development.
Second and Third Trimesters (Week 14 to Delivery):
- The heart rate becomes more regulated.
- The established normal range is 110 to 160 beats per minute.
- The rate will vary within this range, which is a sign of a healthy, responsive nervous system.
Crucial Insight: A single number is less important than the pattern and variability. A healthy heart rate isn’t metronomic; it fluctuates with the baby’s sleep cycles, movements, and even sounds from the outside world. Your provider is listening for this normal fetal heart rate variability.
[Image: https://images.unsplash.com/photo-1559757148-5c350d0d3c56?ixlib=rb-4.0.3 | Caption: A close-up of an ultrasound screen showing the clear, flickering image of a fetal heart during an early pregnancy scan.]
Part 2: Clinical Monitoring: How Healthcare Providers Track the Heartbeat
1. Prenatal Visits: The Fetal Doppler
Starting around 10-12 weeks, your midwife or OB-GYN will begin using a handheld fetal doppler at your checkups.
- How it works: It uses harmless ultrasound waves to detect movement and translates the motion of the heart valves into sound.
- What they’re checking: They note the approximate rate, confirm it’s within the normal range, and listen for a clear, regular rhythm. Finding it can take a moment, depending on the baby’s position, your anatomy, and placental location.
2. The Non-Stress Test (NST)
In the third trimester, especially if a pregnancy is considered high-risk or you go past your due date, you may have non-stress tests.
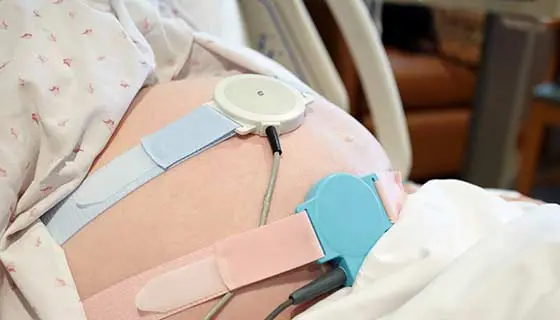
- The Procedure: You recline in a chair with two sensors on your belly—one tracks uterine activity, the other tracks the fetal heart rate. You hold a button to mark when you feel the baby move.
- What it measures: The test looks for accelerations. A healthy, well-oxygenated baby will have temporary increases in heart rate when they move. A “reactive” NST (two or more accelerations in a 20-minute period) is very reassuring.
- Common reasons for an NST: Maternal high blood pressure, diabetes, reduced fetal movement, going past 40 weeks, or concerns about growth.
3. The Biophysical Profile (BPP)
This combines an NST with a detailed ultrasound that scores the baby on five factors: breathing movements, body movements, muscle tone, amniotic fluid volume, and the NST result. The heart rate monitoring is part of this comprehensive check.
4. During Labor: Continuous Electronic Fetal Monitoring (EFM)
In labor, the baby’s heart rate is tracked closely to see how it responds to the stress of contractions.
- External Monitoring: Belly sensors (like an NST) are used.
- Internal Monitoring: If more precise data is needed, a tiny electrode may be placed on the baby’s scalp through the cervix. This gives the most accurate continuous reading.
- Your team watches for reassuring patterns and identifies any non-reassuring patterns that might require a change in the labor plan, like changing position, giving fluids, or in some cases, expediting delivery.
Part 3: The Home Monitoring Dilemma: Fetal Dopplers for Personal Use
The desire to hear that heartbeat at home is completely understandable. Consumer home fetal dopplers are widely sold online. However, this comes with significant cautions.
Potential Risks of Home Use:
- Misidentification: The most common risk. Before 12-14 weeks, it is extremely easy to pick up the sound of your own aortic pulse or placental blood flow, which can sound similar. This gives false reassurance.
- False Reassurance: Hearing a heartbeat does not mean everything is fine. It does not assess fetal well-being, growth, amniotic fluid, or oxygenation. A serious problem could be present even with a “normal” rate you find at home.
- Unnecessary Anxiety: The flip side. If you can’t find the heartbeat—which is common even for professionals due to baby’s position—it can cause panic, even when everything is perfectly okay.
- Delay in Seeking Care: Relying on a home doppler might cause you to delay calling your provider about decreased movement or other concerning symptoms.
If You Choose to Use One: A Responsible Guide
- Wait until at least 12-14 weeks, but know that 16-18 weeks is more realistic for consistent detection.
- Never use it to “check on” the baby in lieu of calling your provider for concerning symptoms (like reduced movement after 28 weeks).
- View it strictly as a bonding experience, not a medical tool.
- Set a time limit. If you don’t find it in 5-10 minutes, stop. Don’t spiral into worry.
[Image: https://images.pexels.com/photos/7550287/pexels-photo-7550287.jpeg | Caption: An expectant couple sharing a quiet, intimate moment, representing bonding without the need for medical devices.]
Part 4: The Gold Standard for Home Awareness: Kick Counting
Starting around 28 weeks, the most important thing you can do daily is track fetal movement, also called kick counting. This is a far more meaningful indicator of well-being than an occasional heart rate check.
Why Movement Matters More: Fetal movement correlates directly with central nervous system health. A baby who moves regularly is generally a healthy baby. A noticeable decrease can be an early warning sign of potential problems.
How to Do a Kick Count:
- Choose a time when your baby is typically active (often after a meal).
- Lie on your side or sit comfortably.
- Count how long it takes to feel 10 distinct movements (kicks, rolls, jabs).
- You should feel 10 movements within 2 hours, though many babies reach 10 in 20-30 minutes.
- Track the pattern daily. It’s the change in your baby’s normal pattern that matters.
If you notice a significant decrease in movement, do not use a doppler. Call your provider immediately. This is the most empowered action you can take.
Part 5: Understanding Concerning Patterns
While interpretation is for medical professionals, it helps to know the basic terms you might hear:
- Tachycardia: A sustained heart rate above 160 BPM. Can be caused by maternal fever, infection, baby’s movements, or medications.
- Bradycardia: A sustained heart rate below 110 BPM. Requires immediate evaluation, especially in labor.
- Decreased Variability: A heart rate that is too steady, with little fluctuation. This can indicate the baby is in a deep sleep cycle (normal) or, if persistent, may signal distress.
- Decelerations: Temporary drops in heart rate. Some are normal and expected with contractions during labor (early decelerations). Others (late or variable decelerations) can be non-reassuring and require intervention.
Conclusion: Trust, Awareness, and Partnership
Tracking your baby’s heart rate is a story of partnership—between you, your baby, and your healthcare team. The technology, from the first flicker on an ultrasound to the continuous monitor in labor, serves one purpose: to ensure a safe journey.
As the parent, your most powerful tools are not devices you can buy, but your own attuned awareness. Paying attention to your baby’s movement patterns is the single best daily practice. Attend your prenatal appointments for professional checks. If you choose to use a home doppler, do so with clear eyes about its limits.
Let the wonder of that heartbeat fill you with joy, not anxiety. Trust in the process, communicate openly with your provider, and know that you are the most connected and important monitor your baby has.
Frequently Asked Questions (FAQ)
Q: My baby’s heart rate was 180 BPM at my 12-week scan. Is that too high?
A: Not necessarily. In the first trimester, heart rates can normally be quite high (peaking around 9-10 weeks) and gradually slow. Your provider will look at the overall context. A rate of 180 BPM at 12 weeks may be at the upper end but is often still within a normal variant, especially if the baby was active.
Q: Does a faster heart rate mean I’m having a girl? (Or a slower rate mean a boy?)
A: No. This is a pervasive old wives’ tale with no scientific basis. Fetal heart rate varies based on gestational age, activity level, and the baby’s own physiology, not biological sex.
Q: What is a normal fetal heart rate during labor?
A: During labor, the normal range is still 110-160 BPM. The focus shifts to how the heart rate responds to contractions. Your care team will look for accelerations and monitor for any decelerations, adjusting your care accordingly.
Q: I’m 34 weeks and my baby’s heart rate dips when I have a Braxton Hicks contraction. Should I worry?
A: Occasional, small decelerations with Braxton Hicks can happen and aren’t automatically concerning. However, you should always report this to your provider at your next visit or call if it’s frequent. They can determine if further evaluation, like an NST, is needed.
Q: Can I feel my own pulse in my stomach and mistake it for the baby’s heartbeat?
A: Absolutely, and this is very common. Your abdominal aorta runs down the center of your body. Its pulse is slower (matching your own resting heart rate of 60-100 BPM) and often feels like a deep, steady thud. The fetal heartbeat is much faster (120-160 BPM) and sounds like a galloping horse under a whooshing sound.
Q: How can I improve fetal heart rate variability?
A: Variability is a sign of a healthy nervous system. Staying hydrated, managing your stress, and maintaining a healthy blood sugar level (especially if you have gestational diabetes) supports a healthy environment for your baby. If you’re concerned about variability on a test, discuss it directly with your provider.

