Pregnancy is a time of profound connection, where every choice you make ripples outward to affect the tiny life growing within you. One of the most powerful protective choices you can make involves modern medicine’s greatest public health achievement: vaccination. Getting the right vaccines during pregnancy isn’t just about safeguarding your own health—it’s about providing your baby with a shield of protection that begins even before their first breath.
This guide will navigate the sometimes-confusing landscape of vaccines during pregnancy. We’ll clearly distinguish between the vaccines that are strongly recommended, those that are advised against, and the ones that depend on your specific situation. Our goal is to move beyond fear and uncertainty, replacing them with evidence-based knowledge. By understanding the “why” behind each recommendation, you can confidently partner with your healthcare provider to make the best decisions for this unique chapter of shared immunity.
Part 1: The Foundational Principle: How Maternal Vaccination Works
To appreciate the power of prenatal vaccines, it helps to understand a bit of brilliant biology. When you receive a vaccine during pregnancy, your immune system does what it’s designed to do: it creates protective antibodies to fight that specific disease.
Here’s the miraculous part: these antibodies don’t stay with you alone. They are actively transferred through the placenta to your developing baby, a process that significantly increases during the late second and third trimesters. This means your baby is born with a temporary, ready-made defense against serious illnesses—a phenomenon called passive immunity.
This is especially crucial because a newborn’s own immune system is immature and doesn’t reach full strength for several months. The antibodies you provide act as a protective bridge, covering them during their most vulnerable early life. It’s one of the first and most profound gifts of health a mother can give.
Part 2: The Core Vaccines: Strongly Recommended During Pregnancy
These vaccines are considered standard of care and are universally recommended by major health organizations like the CDC and ACOG for every pregnancy, regardless of season or prior vaccination history.
1. The Tdap Vaccine (Tetanus, Diphtheria, Pertussis)
- Timing: Recommended during every single pregnancy, ideally between 27 and 36 weeks of gestation. The third-trimester timing maximizes antibody transfer to the baby.
- Primary Purpose: Protecting the Newborn from Pertussis (Whooping Cough). Whooping cough can be life-threatening for infants, causing severe coughing fits that lead to difficulty breathing, pneumonia, and even death. Babies cannot receive their own first dose of the pertussis vaccine until they are 2 months old.
- How it helps: The maternal Tdap vaccine provides the newborn with antibodies to help protect them until they can start their own vaccination series. It’s not about your health as much as it is a direct passive immunization for your baby.
2. The Influenza (Flu) Vaccine
- Timing: Recommended for any trimester during flu season (which is essentially year-round consideration). If you become pregnant during flu season, get vaccinated as soon as possible.
- Primary Purpose: Protecting the Pregnant Person. Pregnancy causes changes to the immune system, heart, and lungs that make you more susceptible to severe illness from the flu. Hospitalization rates are higher for pregnant people with the flu. A high fever from the flu can also pose risks to the developing baby.
- Important Note: You should receive the inactivated flu shot. The nasal spray vaccine (FluMist) contains a live, attenuated virus and is not recommended during pregnancy.
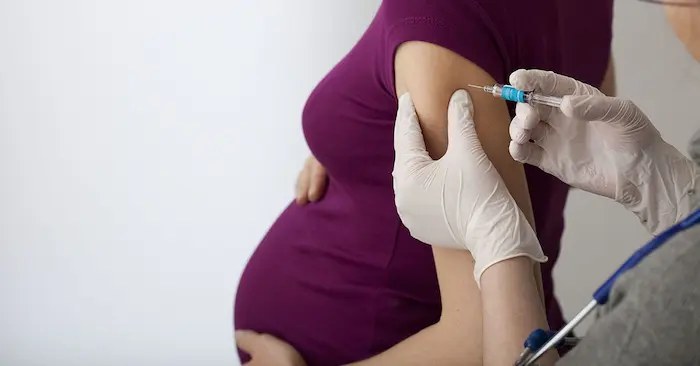
[Image: https://images.unsplash.com/photo-1584467735871-8db9ac8b21c5?ixlib=rb-4.0.3 | Caption: A healthcare professional administers a vaccine to a pregnant woman in a calm, clinical setting.]
3. The COVID-19 Vaccine & Boosters
- Timing: The COVID-19 vaccine is strongly recommended for people who are pregnant, trying to become pregnant, or breastfeeding. Staying up-to-date with recommended boosters is crucial.
- Primary Purpose: Dual Protection. COVID-19 infection during pregnancy significantly increases the risk of severe illness, hospitalization, ICU admission, preterm birth, and other adverse outcomes. Vaccination protects the pregnant person from these severe risks. Furthermore, growing evidence shows that maternal vaccination also provides protective antibodies to the newborn, helping guard them in their first months of life.
Part 3: Vaccines That May Be Recommended Based on Circumstances
These vaccines are not routine for every pregnancy but are advised in specific situations where the risk of disease exposure outweighs the potential risk of the vaccine.
1. Hepatitis B Vaccine
- When it’s recommended: If you are at ongoing risk for Hepatitis B infection (e.g., a healthcare worker, have a partner with Hepatitis B, or have multiple sexual partners) and have not been previously vaccinated.
- Safety: The Hepatitis B vaccine is an inactivated (non-live) virus vaccine, which is considered safe in pregnancy.
2. Special Travel or Exposure Vaccines
If international travel is necessary or you are in an outbreak area, your provider may discuss:
- Hepatitis A Vaccine: Inactivated virus, considered safe if truly needed.
- Meningococcal Vaccine: Also inactivated.
- Rabies Vaccine: Inactivated; crucial if exposed.
- Yellow Fever Vaccine: Contains a live virus. Pregnancy generally contraindicates it unless travel to a high-risk area is unavoidable and the risk of disease is greater than the theoretical risk of the vaccine. This requires a detailed risk-benefit discussion with a travel medicine specialist.
The Golden Rule: Always discuss any planned travel with your obstetrician and a travel clinic well in advance.
Part 4: Vaccines to Avoid During Pregnancy (Live Vaccines)
As a general precaution, vaccines that contain live, attenuated (weakened) viruses are contraindicated during pregnancy due to the theoretical risk of the virus crossing the placenta. The recommendation is typically to wait until after delivery to receive these.
Common live vaccines to postpone:
- MMR (Measles, Mumps, Rubella)
- Varicella (Chickenpox)
- LAIV (Live Attenuated Influenza Vaccine – the nasal spray)
- Yellow Fever (as noted above, used only with extreme caution)
What if I accidentally get a live vaccine while pregnant?
Do not panic. This is a theoretical risk, and there is no documented evidence that these vaccines cause birth defects. The recommendation to avoid them is based on an abundance of caution. Inform your obstetrician, but know that it is not a reason to consider terminating a wanted pregnancy. The Vaccine Pregnancy Registry tracks these exposures to monitor outcomes.
Part 5: Preconception and Postpartum: Closing the Immunity Gaps
Before Pregnancy (The Ideal Time)
The preconception period is the perfect time to ensure you are fully protected. Ask your doctor to check your immunity titers (through a blood test) for:
- MMR: If you are not immune to Rubella, getting vaccinated before conception is vital, as Rubella infection during pregnancy can cause severe congenital disabilities.
- Varicella: Similarly, chickenpox during pregnancy can be dangerous.
Get these live vaccines at least one month before trying to conceive.
Immediately After Delivery (The “Catch-Up” Window)
The postpartum period, especially during your hospital stay or at your first checkup, is a prime opportunity.
- If you never received Tdap or were vaccinated >10 years ago: You can get it postpartum to protect yourself from pertussis and prevent spreading it to your infant.
- If you are not immune to MMR or Varicella: You can and should receive these live vaccines immediately after delivery, even while breastfeeding. Breastfeeding is not a contraindication for any vaccine.
- COVID-19 Boosters: Can be administered postpartum.
- Rhogam: If you are Rh-negative, you will receive this injection after delivery if your baby is Rh-positive.
[Image: https://images.pexels.com/photos/7550287/pexels-photo-7550287.jpeg | Caption: A mother gently holding her newborn's hand, symbolizing the protective bond and shared immunity from vaccination.]
Part 6: Addressing Common Concerns and Questions
Safety and Side Effects
- Are the ingredients safe? Extensive research and surveillance systems (like VAERS and the Vaccine Safety Datalink) continuously monitor the safety of vaccines in pregnancy. The recommended vaccines have not been shown to cause harm to the pregnant person or the fetus.
- Common side effects are mild and similar to those in non-pregnant individuals: a sore arm, low-grade fever, fatigue, or muscle aches for a day or two. These are signs your immune system is responding.
The Question of Autism
This is perhaps the most pervasive myth. There is no credible scientific link between any vaccine (including those given during pregnancy) and the development of autism spectrum disorder. This myth originated from a single, fraudulent study that has been thoroughly retracted and debunked. Major studies involving millions of children have found no association.
What About Mercury (Thimerosal)?
Preservative-free formulations of the Tdap and flu vaccines are available and routinely used for pregnant people. Even if a trace amount of thimerosal (an ethylmercury compound) is present, it is quickly eliminated from the body and has not been shown to cause harm. The fear stems from confusion with methylmercury, a different, harmful compound found in some fish.
Conclusion: An Act of Shared Protection
Navigating the vaccine schedule for pregnancy is fundamentally an act of love—for yourself and for the child you are nurturing. The science is clear and compelling: vaccination is one of the safest, most effective tools we have to prevent serious, sometimes deadly, diseases during a uniquely vulnerable time.
When you receive the Tdap vaccine, you’re not just getting a shot; you’re weaving an invisible cloak of antibodies to drape over your newborn. When you get your flu shot, you’re fortifying your own health so you can be strong and present for the journey ahead. Have open conversations with your provider. Voice your concerns. Review the evidence together.
In a world of so many uncertainties, this is a powerful step you can take with confidence. It’s a proactive choice for health, embodying the profound truth that in pregnancy, caring for yourself is the very foundation of caring for your baby.
Frequently Asked Questions (FAQ)
Q: I got a Tdap shot in my last pregnancy. Do I really need it again?
A: Yes, during every pregnancy. Antibody levels peak and then decline. Getting Tdap with each pregnancy ensures each newborn receives the highest possible level of protective antibodies during their most vulnerable period.
Q: Can I get the RSV vaccine while pregnant?
A: As of recent guidelines (2023), yes. A new maternal RSV vaccine (Abrysvo) is recommended for pregnant people during weeks 32 through 36 of pregnancy, from September through January, to protect infants from severe RSV illness after birth. This is a major new tool in infant protection. Always confirm the latest recommendations with your provider.
Q: I’m pregnant and not sure if I had the chickenpox vaccine or the disease. What should I do?
A: Inform your provider. They can order a simple blood test to check your varicella immunity status. If you are not immune, you will be counseled to avoid exposure and will receive the vaccine postpartum.
Q: Are vaccines given during pregnancy safe if I’m breastfeeding?
A: Absolutely. All routine vaccines (COVID-19, flu, Tdap, MMR, varicella) are safe and recommended during breastfeeding. The antibodies you produce can also pass into your breast milk, providing an additional layer of protection for your baby.
Q: What if I have a severe egg allergy? Can I get the flu shot?
A: Yes. Most flu vaccines today contain such tiny, trace amounts of egg protein that the CDC recommends vaccination for people with egg allergies in any setting. If you have a history of a severe reaction (e.g., anaphylaxis) to eggs, the vaccine can be given under the supervision of a healthcare provider who can manage allergic conditions.
Q: I’m in my first trimester and just found out I’m pregnant. Is it too late for vaccines?
A: It’s not too late, but timing is optimized. The flu and COVID-19 vaccines can be given in any trimester. For Tdap, you will wait until the recommended 27-36 week window to maximize antibody transfer for pertussis protection. Discuss your specific schedule with your provider at your first prenatal visit.

