Picture this: you’re settled into your favorite nursing chair, and your baby is rooting hungrily. You gently guide them to your breast, but instead of a sweet bonding moment, you feel it—a sharp, shooting pain that literally takes your breath away. Maybe it’s the sting of cracked skin that makes every latch feel like sandpaper, or perhaps it’s a deep, heavy ache that lingers long after your baby has finished eating. You might even be dealing with random zaps of pain that leave you feeling anxious about the next feeding session.

If any of this resonates with you, please know that you are not alone—and most importantly, you do not have to just “tough it out.”
While breastfeeding is a natural process, that doesn’t mean it’s always easy or pain-free right out of the gate. It’s normal to feel some mild tenderness in those first few days while you and your baby are still finding your rhythm. However, persistent, sharp, or worsening pain is your body’s way of telling you that something needs a little extra attention. It isn’t just “part of the job.”
The good news is that most causes of breastfeeding discomfort are completely treatable. With the right support and a bit of knowledge, you can move away from dreading feedings and get back to the comfortable, connected experience you envisioned.
This guide is designed to help you figure out exactly what’s going on based on where and how it hurts. We’ll look at common causes, evidence-based solutions, and exactly when it’s time to call in a professional so you can heal and feel like yourself again.
Understanding Breastfeeding Pain: What’s Normal and What’s Not
When you’re new to nursing, it can be hard to tell the difference between “learning curves” and actual problems. Let’s break down the typical sensations versus the red flags.
Normal Sensations in Early Breastfeeding
As your body adjusts during the first couple of weeks, you might notice:
- Latch-on sensitivity: A brief “toe-curling” moment when the baby first latches that usually fades within 30 to 60 seconds.
- A gentle tugging: A distinct pulling feeling as the baby draws milk, which shouldn’t feel sharp.
- The “Let-Down” feeling: A tingly, pins-and-needles sensation or a sudden rush of fullness when your milk starts flowing (though some moms don’t feel this at all!).
According to the American Academy of Pediatrics (AAP), while some initial adjustment is common, breastfeeding should never cause pain that lasts throughout the entire nursing session.
Red Flags: When Pain Signals a Problem
It’s time to take a closer look if you experience any of the following:
- Sharp or burning pain that continues the whole time the baby is sucking.
- Pain between feedings that just doesn’t seem to let up.
- Nipples that are cracked, bleeding, or blistered.
- Fever or flu-like symptoms (like chills, aches, and extreme fatigue) paired with breast pain.
- A specific area on the breast that feels red, hot, and very tender to the touch.
- Nipples that look white or purple immediately after the baby unlatches.
- A feeling of dread when you know it’s time to nurse again.
The experts at the Mayo Clinic emphasize that persistent pain is a signal to seek help so you can address the root cause and get back to comfort.
Common Causes of Breastfeeding Pain
Because “breast pain” can mean many things, identifying exactly where and how it hurts is the first step toward fixing it.
Nipple Pain
Shallow Latch and Improper Positioning
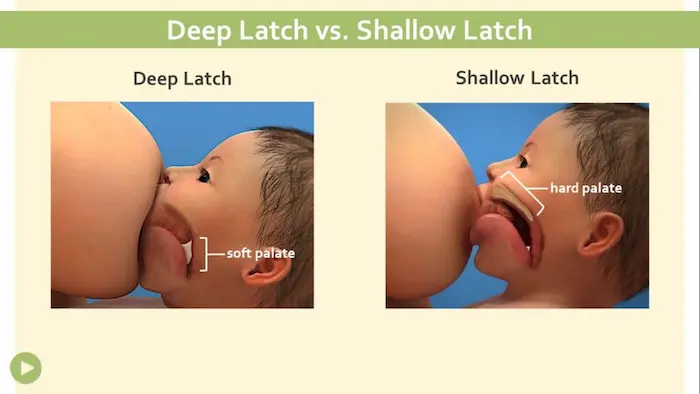
What it is: This happens when the baby is only “nippling”—sucking on the tip rather than taking in a good mouthful of breast tissue. Instead of the nipple resting safely against the soft palate in the back of the mouth, it gets rubbed or pinched against the baby’s hard palate or tongue.
What it feels like: A pinching or sharp sensation throughout the feed. When the baby unlatches, your nipple might look flattened, slanted, or shaped like a new tube of lipstick.
Why it happens: It’s usually a matter of positioning, rushing the latch, or the baby not opening their mouth wide enough. Sometimes, physical factors like a tongue-tie can also play a role.
Nipple Trauma (Cracks, Blisters, or Bleeding)
What it is: Actual physical damage to the nipple skin, often caused by the friction of a poor latch or an incorrectly fitted breast pump.
What it looks like: You might see visible cracks, scabbing, or even small blisters. The pain often lingers even when you aren’t nursing.
Why it happens: A shallow latch is the most common culprit, but using a pump flange that is too small or too large can also cause significant damage.
Thrush (Yeast Infection)
What it is: An overgrowth of yeast (Candida) that can infect both your nipples and the milk ducts inside the breast.
What it feels like: A burning, stabbing, or “shooting” pain deep within the breast that often intensifies after a feeding. Your nipples might look unusually shiny, flaky, or bright pink.
What it looks like in baby: Check your baby’s mouth for creamy white patches on the tongue or cheeks that don’t wipe away. They may also have a persistent, angry red diaper rash.
Why it happens: Yeast loves warm, moist environments. It often crops up after you or the baby have finished a course of antibiotics, or if your skin is already compromised by cracks.
Vasospasm and Raynaud’s Phenomenon
What it is: This occurs when the blood vessels in the nipple constrict suddenly, cutting off blood flow. It’s often triggered by a drop in temperature or the trauma of a poor latch.
What it looks like: This is very distinct—after the baby unlatches, the nipple tip turns white (blanches), then may turn blue or purple, and finally bright red as the blood rushes back in.
What it feels like: A throbbing or burning sensation that can be quite intense and can last for a while after the feeding is over.
Why it happens: It’s a reaction to cold air hitting the nipple or a response to the nipple being compressed during a shallow latch.
Nipple Blanching
What it is: Physical compression during nursing that squeezes the blood out of the nipple tip.
What it looks like: The nipple looks flattened and pale white immediately after a feed, often with a visible “line” where it was squeezed.
What it feels like: A painful burning or throbbing as the blood flow returns to the area.
Why it happens: Usually, this is due to the baby’s mouth position or the way they are using their tongue/jaw to hold onto the breast.
Milk Blisters (Blebs)
What it is: A tiny, painful white or yellow spot on the tip of the nipple. It’s essentially a tiny bit of skin that has grown over a milk duct, causing milk to back up behind it.
What it feels like: A very sharp, localized “pinprick” pain, especially right when your milk lets down.
Why it happens: These can be caused by a shallow latch, an oversupply of milk, or even a bra that fits too tightly.
Breast Pain
Engorgement
What it is: When your breasts become overly full of milk and fluid, leading to swelling and firmness.
What it looks like: Your breasts might look shiny, feel hard to the touch, and seem much larger than usual. The swelling can sometimes make the nipple so flat that the baby has trouble latching on.
What it feels like: A heavy, throbbing, or aching pain throughout the entire breast.
Why it happens: This is most common when your milk “comes in” (around days 3-5), but it can also happen if you miss a feeding or if the baby isn’t effectively removing milk.
Plugged (Clogged) Ducts
What it is: Milk that gets “stuck” in a specific duct, causing a backup and inflammation.
What it looks like: You’ll likely feel a small, tender lump in one area of your breast. The skin over the lump might look slightly pink or red.
What it feels like: Localized soreness that usually feels worse before a feeding and better after the baby drains that area.
Why it happens: This can be caused by skipped feedings, a bra that’s too tight, or even sleeping in a position that puts pressure on one part of the breast.
Mastitis
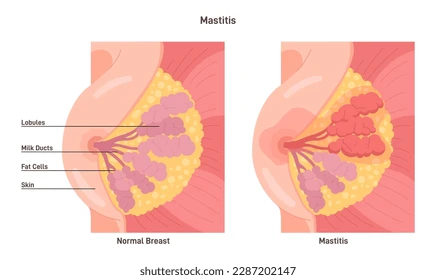
What it is: An inflammation of the breast tissue that often leads to an infection. It can happen when a clogged duct is left untreated or when bacteria enters through a cracked nipple.
What it looks like: A wedge-shaped area of redness that feels hot, swollen, and very painful.
What it feels like: Intense pain accompanied by a fever, chills, and total body exhaustion—essentially, you feel like you have the flu.
Why it happens: When milk stays stagnant in the breast, it allows bacteria to grow. It’s your body’s way of saying it needs rest and medical help.
Important: Mastitis is a medical issue. If you feel flu-like symptoms along with breast pain, please reach out to your doctor immediately.
Inflammatory Conditions (Rare)
While extremely rare, any persistent, unexplained breast pain or skin changes should be checked by a professional. This isn’t meant to worry you, but rather to ensure that any unusual symptoms are ruled out quickly by a doctor.
Deep Breast Pain
Let-Down Pain
What it is: This is the physical sensation of milk moving from the small sacs (alveoli) into your milk ducts.
What it feels like: While many women find it barely noticeable, some feel a strong tingling. However, if it feels like an intense shooting pain, it might be related to:
- An overactive let-down: Milk that sprays too forcefully.
- Thrush: Which can turn a normal let-down into a stinging sensation.
- D-MER: A rare condition where milk release triggers a sudden wave of negative emotions, though this is emotional rather than physical pain.
Mondor’s Disease
What it is: A rare inflammation of a vein just beneath the skin of the breast.
What it looks like: You might notice a tender, cord-like lump under the skin.
What it feels like: Sensitivity and soreness along that specific “cord.” It usually resolves on its own but is worth mentioning to your doctor.
Latch and Positioning: The Foundation of Comfortable Breastfeeding
Since the vast majority of breastfeeding pain starts with the latch, getting back to the basics can often solve the problem almost instantly.
Signs of a Great Latch
A comfortable, effective latch should look like this:
- Asymmetry: The baby has more of the bottom part of your areola in their mouth than the top.
- Chin in: The baby’s chin is pressed firmly into your breast.
- Nose clear: Their nose might touch the breast, but they should be able to breathe easily.
- “Fishy” lips: Both the top and bottom lips should be flanged outward, not tucked in.
- Rounded cheeks: You shouldn’t see any dimples or “sucking in” of the cheeks.
- Full jaw movement: You can see the rhythm of their jaw moving all the way back to their ears.
- Peace of mind: Most importantly, you should feel comfortable!
Common Positioning Pitfalls
- The “Twist”: If the baby’s head is turned to the side but their body is facing up, it makes swallowing and latching difficult. Keep them “tummy to mommy.”
- The Hunch: Don’t lean forward to find the baby. Use pillows to bring the baby up to your breast level so you can sit back and relax.
- Head pressure: Pushing on the back of the baby’s head often makes them arch away. Instead, support them at the base of the skull or neck.
- The Rush: Trying to latch before the baby’s mouth is wide open (like a big yawn) almost always results in a shallow, painful latch.
Getting Support
If you’re struggling, please don’t hesitate to reach out to a lactation consultant. They are like “breastfeeding coaches” who can watch a full feeding and give you hands-on tips that make a world of difference. You can also find wonderful, free support through local La Leche League groups.
Solutions for Nipple Pain
Fixing the Latch
- Always check that your baby is well-aligned (nose to nipple, tummy to tummy).
- Wait for a “big yawn” before bringing the baby to the breast.
- Don’t be afraid to unlatch and try again if it doesn’t feel right. (Use your pinky to gently break the suction first!)
Healing Damaged Nipples
For immediate relief:
- Liquid gold: Express a little breast milk and rub it on your nipples after feeding; its natural properties are incredibly healing.
- Lanolin: A thin layer of medical-grade lanolin can help protect the skin.
- Hydrogel pads: These are a lifesaver for severe cracks, providing a cooling sensation and helping wounds heal faster.
- Fresh air: Whenever possible, let your nipples air dry between feedings.
Managing Thrush
Because thrush is an infection, you and your baby usually need to be treated at the same time to stop you from passing it back and forth. Your doctor may prescribe an antifungal cream for you and a gel or drops for the baby. Make sure to sterilize any pump parts, pacifiers, or bottle nipples daily until the infection is cleared.
Dealing with Vasospasm
The key here is warmth. Try covering your breast immediately after the baby unlatches so the cold air doesn’t trigger a spasm. Some moms find that a dry, warm compress held against the breast right after nursing provides huge relief.
Soothing Milk Blisters
Before you nurse, try applying a warm, wet washcloth to the area to soften the skin. Gently rubbing the spot with the cloth after a feed can sometimes help the blister clear naturally. If it doesn’t go away, a professional can help you safely open it—don’t try to pop it yourself!
Solutions for Breast Pain
Relieving Engorgement
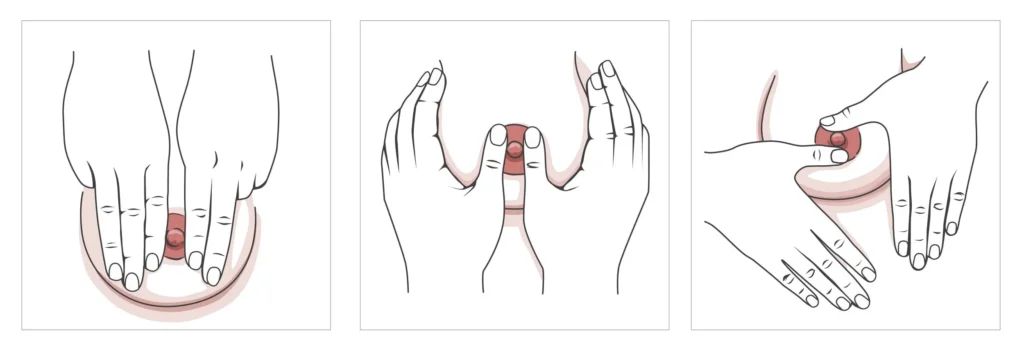
If your breasts are so full that your baby can’t latch, try reverse pressure softening. Use your fingertips to gently press the tissue around the base of the nipple inward for about a minute. This moves the swelling back and makes the nipple soft enough for the baby to grab. Between feedings, a cold compress or even chilled cabbage leaves can help bring down the inflammation.
Clearing Plugged Ducts
The most important thing is to keep the milk moving. Nurse frequently on the affected side and gently massage the lump toward the nipple while the baby is feeding. Applying heat just before you nurse can help the milk flow more easily, but use cold after nursing to soothe the area. Also, make sure you aren’t wearing anything that constricts your breasts!
Treating Mastitis
If you suspect mastitis, call your doctor. You will likely need a course of antibiotics. While you heal, it is crucial that you keep breastfeeding or pumping on the affected side. Your milk is perfectly safe for the baby, and emptying the breast is the best way to clear the infection. Get as much rest as you possibly can—your body needs it to fight the infection.
When to See a Doctor or Lactation Consultant
Knowing when to call for help can prevent a small issue from becoming a major hurdle.
Red Flags: Call Your Doctor If:
- You have a fever over 101°F (38.3°C).
- You feel like you have the flu (chills, body aches).
- You see red streaks extending across your breast.
- The pain is getting worse despite your efforts at home.
- A lump doesn’t soften or disappear after nursing and massage.
Who to Call for What
Lactation Consultants (IBCLC) are your go-to for anything related to the “act” of breastfeeding—latch, positioning, and milk transfer. Doctors (OB/GYN) are the experts for treating infections like mastitis or thrush and managing any necessary medications.
Self-Care While Healing
Nursing through pain is physically and emotionally exhausting. While you’re working on a solution, don’t forget to take care of yourself.
Pain Management
Over-the-counter pain relievers like acetaminophen (Tylenol) or ibuprofen (Advil/Motrin) are generally considered safe for breastfeeding moms and can help manage inflammation. Always double-check with your provider first, but don’t feel guilty about taking something to help you manage the discomfort.
Emotional Support
Breastfeeding struggles can feel very isolating. Reach out to a friend who has been there, join an online support group, or just talk to your partner about how you’re feeling. Seeking help isn’t a sign of failure—it’s a sign that you are a dedicated parent doing whatever it takes to make this work for you and your baby.
Frequently Asked Questions
Why does my breast hurt after feeding?
Post-feed pain is often due to lingering engorgement, a vasospasm (the nipple reacting to the air), or potentially a yeast infection (thrush) which typically causes a deep, burning ache after the baby unlatches.
Can I continue breastfeeding with mastitis?
Yes, and you should! Continuing to move milk through the affected breast is one of the most important parts of the healing process. Your milk contains antibodies that are safe for your baby, and keeping the duct clear is vital.
How do I know if I have thrush or just sore nipples?
Thrush pain usually feels like a deep burning or “shooting” sensation that doesn’t go away even with a perfect latch. If your nipples look shiny or pink and your baby has white patches in their mouth, it’s likely thrush.
Is it safe to take pain medication while breastfeeding?
Common options like Tylenol and Advil are widely considered safe for nursing mothers. Always check with your doctor or pharmacist to be sure, especially if your baby was born prematurely.
Will pumping instead of nursing help with pain?
It can give your nipples a temporary “break” from a painful latch, but it’s not always a perfect fix. If your pump flange doesn’t fit correctly, it can cause its own set of problems. It’s best to work with a consultant to find a balance that allows you to heal.
Why do I have shooting pains in my breast?
These “zaps” are often just your let-down reflex, but if they are very painful, they could be a sign of thrush, a vasospasm, or a clogged duct that is starting to clear.
Can I prevent breastfeeding pain?
The best prevention is getting help with your latch as early as possible. Feed your baby whenever they show hunger cues, change up your nursing positions, and make sure you aren’t wearing restrictive clothing.
Conclusion
If you’re reading this while in pain, please take a deep breath. You are doing a wonderful job, and you’ve already taken the most important step by looking for answers.
The most important thing to remember is this: breastfeeding is not supposed to be a painful endurance test. Almost every cause of discomfort has a solution. Whether it’s a quick adjustment to your baby’s position or a short course of treatment for an infection, you can get back to a place where nursing feels like the sweet, bonding experience you deserve.
Be gentle with yourself, reach out for support when you need it, and know that things will get better. You and your baby are a team, and with a little help, you’ll find your rhythm soon.

