Imagine having the ability to peek into your baby’s genetic blueprint with nothing more than a simple blood draw. No needles near your belly, no medical procedures, just a routine vial of blood that could reveal crucial information about your baby’s health. This is the promise of Non-Invasive Prenatal Testing (NIPT), one of the most significant advances in modern prenatal care.
First introduced in 2011, NIPT has transformed how expectant parents approach genetic screening. It’s moved from being a specialized test for high-risk pregnancies to a mainstream option offered to virtually all pregnant individuals. But with this accessibility comes important questions: What exactly does it test for? How accurate is it really? And most importantly, should you get it?
This guide will walk you through everything you need to know about NIPT—not as a sales pitch, but as a balanced, thorough resource. We’ll explore the science behind the test, discuss what it can and cannot tell you, and provide you with the questions to ask your healthcare provider. By the end, you’ll have the knowledge to make an informed, confident decision about whether NIPT aligns with your values and needs for this pregnancy.
Part 1: Demystifying NIPT – What Is It and How Does It Work?
The Simple Blood Test with Complex Science
At its core, NIPT (also called NIPS – Non-Invasive Prenatal Screening) is a sophisticated maternal blood test. What makes it revolutionary isn’t the blood draw itself, but what scientists can now detect in that blood.
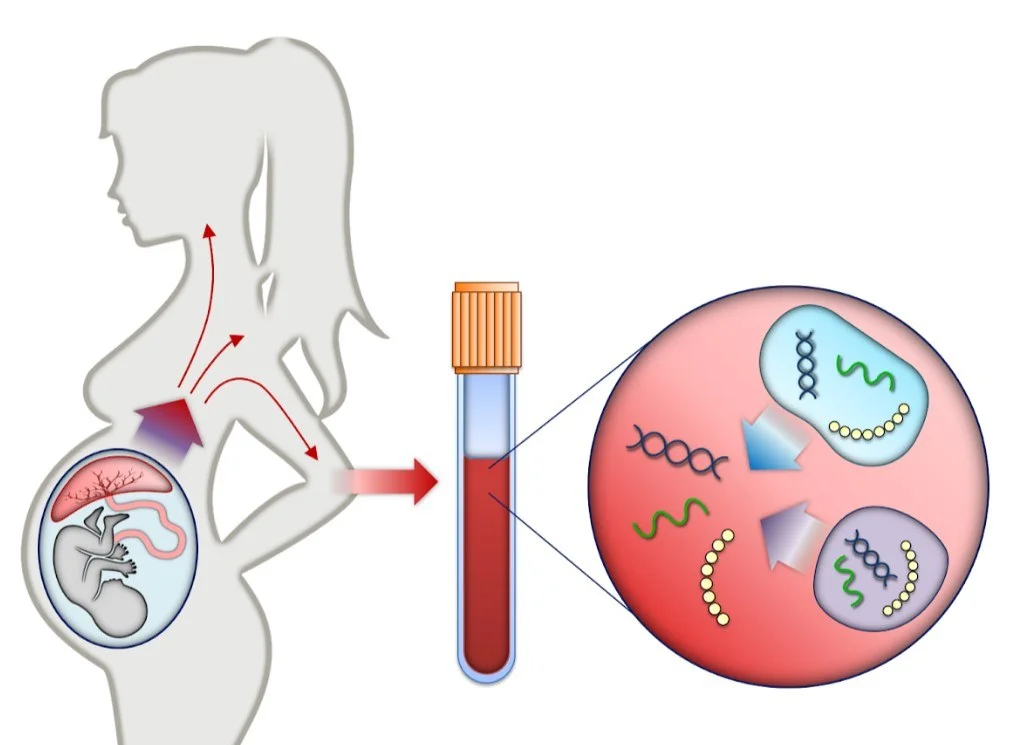
During pregnancy, your bloodstream contains a mix of your own DNA and small fragments of DNA from the placenta, known as cell-free fetal DNA (cffDNA). These placental DNA fragments are virtually identical to the baby’s DNA. NIPT uses advanced sequencing technology to analyze this genetic material.
The Analogy: Think of it like finding puzzle pieces from two different boxes mixed together. Scientists have become incredibly skilled at separating “mom’s puzzle pieces” from “baby’s puzzle pieces” and then checking if the baby’s pieces show any extra or missing chromosomes.
What Does NIPT Actually Screen For?
It’s crucial to understand that NIPT is a screening test, not a diagnostic test. It assesses risk, it doesn’t give definitive yes/no answers. Here’s what most standard NIPT panels screen for:
- The Major Trisomies (Primary Focus):
- Down Syndrome (Trisomy 21): An extra copy of chromosome 21.
- Edwards Syndrome (Trisomy 18): An extra copy of chromosome 18.
- Patau Syndrome (Trisomy 13): An extra copy of chromosome 13.
- Sex Chromosome Conditions:
- Conditions like Turner syndrome (Monosomy X) or Klinefelter syndrome (XXY).
- Fetal Sex Determination: NIPT can accurately predict the baby’s biological sex by detecting the presence or absence of a Y chromosome.
- Optional/Expanded Panels:
Some labs offer tests that also screen for:- Microdeletions: Small missing pieces of chromosomes (e.g., 22q11.2 deletion syndrome, which causes DiGeorge syndrome).
- Rarer Trisomies: Involving other chromosomes.
[Image: https://images.unsplash.com/photo-1551601651-2a8555f1a136?ixlib=rb-4.0.3 | Caption: A phlebotomist gently drawing a blood sample from a patient's arm, representing the simple, non-invasive nature of the NIPT blood test.]
Part 2: The Numbers Game – Understanding NIPT Accuracy
When evaluating “NIPT test accuracy,” you’ll encounter specific terms: detection rate and false positive rate. Let’s break these down with real numbers.
Detection Rates (Sensitivity)
This is the test’s ability to correctly identify a pregnancy that does have the condition.
- Down Syndrome (T21): >99% detection rate. This means it catches over 99 out of 100 actual cases.
- Edwards Syndrome (T18): >97% detection rate.
- Patau Syndrome (T13): Around 90% detection rate.
- Fetal Sex: Over 99% accurate when fetal fraction is sufficient.
False Positive Rates
This is the chance the test will indicate a high risk when the baby does not actually have the condition.
- Extremely Low: Generally less than 0.1% (less than 1 in 1,000) for the main trisomies. This is a key advantage over traditional serum screenings, which had false positive rates around 5%.
The Critical Concept: Fetal Fraction
For NIPT to work, there must be enough placental DNA in your blood sample. This is called the fetal fraction. A minimum threshold (usually 3-4%) is required for an accurate result.
Factors that can lead to low fetal fraction:
- Testing too early (before 10 weeks)
- High maternal weight/obesity
- Certain medical conditions
A “low fetal fraction result” does not mean something is wrong. It simply means the test couldn’t get a clear read. Your provider will typically recommend a redraw in 1-2 weeks. Persistently low fetal fraction can be associated with certain chromosomal conditions or placental issues, which your provider will discuss with you.
Part 3: Who is NIPT For? Understanding the Guidelines
The Shift from High-Risk to All Pregnancies
Initially, NIPT was recommended primarily for pregnancies with:
- Advanced maternal age (35 or older at delivery)
- Previous pregnancy with a chromosomal condition
- Abnormal traditional screening result
- Certain ultrasound findings
However, major medical societies now state that NIPT can be offered to all pregnant individuals as a primary screening option, regardless of age or risk factors. The high accuracy and low false positive rate make it a compelling choice for anyone seeking early information.
Special Considerations: Twins and IVF Pregnancies
- Twins: NIPT is available for twin pregnancies, but accuracy is slightly lower, especially for identifying which twin is affected. It cannot screen for twin-to-twin transfusion syndrome.
- IVF Pregnancies: NIPT works well, but it’s essential your provider knows if you used an egg donor, as the test will detect the donor’s DNA profile, not yours.
Part 4: The Decision Matrix – Key Factors to Consider
Reasons You Might Choose NIPT
- Early and Accurate Information: You can get results as early as 10-12 weeks, giving you more time to process information and make decisions.
- Peace of Mind: For many, the high accuracy and low false positive rate provide significant reassurance, especially if they’re anxious about chromosomal conditions.
- Avoiding Unnecessary Invasive Procedures: Because NIPT has such a low false positive rate, it can prevent many people from undergoing unnecessary amniocentesis or CVS, which carry a small miscarriage risk.
- Planning and Preparation: If there is a high-risk result, families have more time to prepare—medically, emotionally, and logistically—for a child who may have special needs.
- Knowing Fetal Sex Early: While not a medical reason, this is a motivating factor for some families.
Reasons You Might Decline or Postpone NIPT
- Cost and Insurance Coverage: This is the biggest practical barrier. While many insurers now cover it for women over 35, others may not. Out-of-pocket costs for NIPT can range from $99 to over $2,000. Always verify with your insurance and ask the testing company about self-pay options.
- “It’s Just a Screen” Mindset: You may feel that since it’s not diagnostic, you’d prefer to wait for your anatomy ultrasound (18-20 weeks) or skip genetic screening altogether.
- Anxiety vs. Reassurance: For some, any screening causes anxiety. You might worry about ambiguous results, low fetal fraction, or what you’d do with a high-risk result.
- Ethical Considerations: Some parents feel they would continue the pregnancy regardless of findings and prefer not to have the information, avoiding potential psychological burden or implicit bias during pregnancy.
- Content with Traditional Screening: You may opt for the first-trimester combined screen or quad screen, which are less expensive (though less accurate) and may be fully covered.
[Image: https://images.unsplash.com/photo-1579684385127-1ef15d508118?ixlib=rb-4.0.3 | Caption: A thoughtful conversation between a doctor and expectant parents, representing the shared decision-making process about prenatal testing.]
Part 5: The Reality of Results: What Comes Next?
Receiving a Low-Risk Result
This is the most common outcome. A low-risk result means the chance your baby has the screened-for conditions is very low. However, it is not a guarantee. NIPT does not screen for all birth defects, genetic conditions, or complications. You should still complete your anatomy ultrasound and all recommended prenatal care.
Receiving a High-Risk or Positive Result
This can be emotionally overwhelming. The first thing to remember: Do not make any irreversible decisions based on NIPT alone. A high-risk NIPT result is not a diagnosis.
The next steps are:
- Genetic Counseling: You will be referred to a genetic counselor who will explain the result in detail, the specific condition, and your options.
- Diagnostic Testing: To get a definitive answer, you will be offered a diagnostic test—either Chorionic Villus Sampling (CVS) or amniocentesis. These procedures analyze actual fetal cells and can confirm or rule out the condition with near 100% accuracy.
- Detailed Ultrasound: A specialist will perform a targeted ultrasound to look for physical markers associated with the suspected condition.
Part 6: The Critical Conversation – Questions for Your Provider
Before deciding, bring these questions to your prenatal visit:
- “Which specific NIPT lab do you use, and what conditions does their panel screen for?”
- “What is your experience with NIPT false positive stories or low fetal fraction results?”
- “Can you help me understand my likely insurance coverage for NIPT, and what are my self-pay options?”
- “If my result is high-risk, what is your protocol? How quickly can I see a genetic counselor?”
- “Regardless of my NIPT result, what other screenings (like the neural tube defect screen) will I still need?”
Conclusion: Information as Power, Choice as Freedom
The decision about whether to get NIPT during pregnancy is deeply personal. There is no universally “right” answer. For some, the early, accurate information is invaluable for peace of mind and preparation. For others, the cost or the emotional weight of potential results makes it less appealing.
What matters most is that you make the choice from a place of understanding. NIPT is a powerful tool, but it’s just one piece of your prenatal care puzzle. It provides specific genetic risk information, but it doesn’t measure your baby’s heart development, organ formation, or your own maternal health.
Whether you choose NIPT or not, remember that the ultimate goal is a healthy pregnancy and a supported transition to parenthood. Have the conversation with your provider, discuss it with your partner, and trust yourself to choose the path that brings you the most confidence and calm on your unique journey.
Frequently Asked Questions (FAQ)
Q: How is NIPT different from the first-trimester screen?
A: The first-trimester screen combines a blood test (PAPP-A, hCG) with an ultrasound measurement of the baby’s nuchal translucency (NT). It has about an 85-90% detection rate for Down syndrome with a 5% false positive rate. NIPT uses only a blood test but analyzes fetal DNA directly, offering >99% detection with a <0.1% false positive rate for T21.
Q: Can NIPT tell me if my baby has autism or intellectual disability?
A: No. NIPT only screens for specific chromosomal abnormalities. Autism and most intellectual disabilities have complex causes not related to the whole-chromosome conditions NIPT detects.
Q: I’m under 35 and low-risk. Is NIPT worth it for me?
A: This is a personal value decision. While your baseline risk is lower, chromosomal conditions can occur in any pregnancy. The high accuracy of NIPT may provide extra reassurance. The main consideration is often cost versus your desire for that early, highly accurate information.
Q: What does “no result” or “test failure” mean on an NIPT report?
A: This is usually due to low fetal fraction. It’s not a reflection of your baby’s health. You’ll typically be asked to repeat the test in 1-2 weeks. In some cases, persistent low fetal fraction can be associated with placental issues or, rarely, maternal malignancy, which your doctor will investigate.
Q: How long does it take to get NIPT results?
A: Typically 7-14 calendar days from when the lab receives your blood sample. Some labs offer expedited options.
Q: If my NIPT is low-risk, do I still need the 20-week anatomy scan?
A: ABSOLUTELY YES. The anatomy ultrasound is crucial for checking your baby’s physical development—brain, heart, spine, kidneys, limbs, etc. NIPT does not screen for structural birth defects, which are often detected at the 20-week scan. The two tests provide completely different, complementary information.

