Congratulations! That positive test result has likely sent a whirlwind of emotions through you excitement, disbelief, and maybe a touch of anxiety. Welcome to the incredible, and often challenging, journey of the first trimester. Those initial twelve weeks are a period of profound, rapid change, both for your growing baby and for you. If you’re feeling overwhelmed by symptoms, uncertainty, or a barrage of online information, take a deep breath. You’ve just found your compassionate, week-by-week companion. This guide is designed not just to inform you, but to support you. We’ll navigate the common hurdles, celebrate the milestones, and equip you with practical first trimester survival tips to help you not just endure, but thrive.

Think of this as a roadmap from those very first whispers of pregnancy through the exciting end of the first chapter. We’ll dive into what’s happening inside your body each week, tackle symptoms head on with actionable strategies, and answer the questions that keep you up at night. Whether you’re searching for “6 weeks pregnant what to expect” or wondering how to handle “managing morning sickness at work,” we’ve got you covered. Let’s begin.
Understanding Your First Trimester: More Than Just Symptoms
The first trimester spans weeks 1 through 12 of pregnancy (yes, it starts from the first day of your last period—a confusing but important detail!). This is the most critical period of fetal development. Your body is engineering a placenta and building the foundation of every single organ system in your baby’s body. It’s a monumental task, and the hormonal surge powering this project—hello, hCG and progesterone is largely responsible for the symptoms you feel.
This is why extreme fatigue in early pregnancy isn’t just “being tired.” It’s your body’s direct request for you to slow down and redirect energy to the incredible work happening within. Recognizing this can transform how you view these challenges. They are signs of a process unfolding exactly as it should, even when it feels uncomfortable.
Your Week-by-Week Guide: From Poppy Seed to Lime
Let’s break down these early weeks. Focusing on specific weeks can provide the reassurance you’re looking for when general advice feels too vague.
Weeks 5-8: The Foundation Forms
This is often when reality sets in, thanks to both a missed period and the arrival of early symptoms.
- Week 5: Your baby is now the size of a sesame seed. The neural tube, which will become the brain and spinal cord, is forming. You might start noticing tender breasts, mild fatigue, or a newfound aversion to certain smells. It’s a common time for first suspicions.
- Week 6: What to Expect. This is a big one. Your baby’s heart, though tiny, begins to beat and might even be visible on an early ultrasound. Little buds that will become arms and legs appear. For you, symptoms often ramp up. Nausea (which, let’s be honest, can strike any time of day) may begin. You might feel bloated or experience mild cramping as your uterus expands. The key here is to listen to your body. If all you can stomach is crackers and lemon water for a few days, that’s perfectly okay.
- Week 7: Features are starting to take shape with dark spots for eyes and nostrils. The arm and leg buds are growing longer. You may find your sense of smell is almost superhero-level strong, and coping with pregnancy anxiety might feel more pressing as symptoms intensify.
- Week 8: Your baby graduates from embryo to fetus! Webbed fingers and toes are forming. This week, the extreme fatigue can be profound. It’s normal to need a nap after simple tasks. This is your body’s clear instruction to rest.
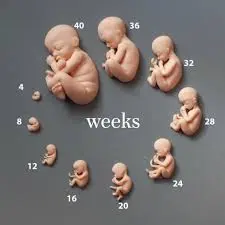
Weeks 9-12: The Transition Phase
As you near the end of the first trimester, many women start to feel a subtle shift.
- Weeks 9 & 10: The fetus is now about the size of a grape. Vital organs like kidneys and intestines are starting to function. For you, nausea may peak around week 9. Your waistline might begin to soften as your uterus grows to the size of a large orange.
- Week 11: Your baby is officially developing bones and tiny tooth buds. You might notice your hair and nails growing faster thanks to increased blood flow and hormones. Some women see a slight abatement in nausea.
- Week 12: A major milestone! Your baby’s reflexes are developing—they might start to squirm, though you won’t feel it yet. Your uterus rises above your pelvic bone, which can mean a slight decrease in bladder pressure (fewer nightly bathroom trips!) and, for many, the beginning of the end of constant nausea. The risk of miscarriage drops significantly, offering many parents-to-be a deep sense of relief.
Conquering Common First Trimester Challenges: Your Survival Toolkit
Knowledge is power, but practical strategies are your lifeline. Here are battle-tested tips for navigating the most common hurdles.
1. Taming the Nausea Beast
“Morning sickness” is a misnomer. It can strike any time. The key is prevention and gentle management.
- The 5-Minute SOS Routine for Sudden Nausea: Keep a “survival kit” by your bed and at work. At the first wave, 1) Suck on a pre-frozen lemon wedge or sour candy. 2) Sniff a drop of peppermint or lemon essential oil on a handkerchief. 3) Sip small, cold sips of ginger ale or plain carbonated water. The combination of sour, scent, and sip can often short-circuit the nausea signal.
- Managing Morning Sickness at Work: Be strategic. Keep bland snacks (pretzels, almonds, crackers) in your desk drawer and nibble every hour. A small fan at your desk can help with stuffiness or food odors. Have a discreet conversation with your manager if needed—most are understanding. Hydrate with ice-cold water or electrolyte popsicles.
2. Navigating Extreme Fatigue
This isn’t ordinary tiredness. It’s a deep, bone-weary exhaustion.
- Listen and Obey: If your body says nap, try to nap. Even a 20-minute power nap can reset your system.
- Micro-Nutrition: Ensure you’re getting enough iron and protein. Pair iron-rich foods like spinach with vitamin C (like bell peppers) for better absorption. Small, frequent meals stabilize blood sugar, preventing energy crashes.
- Delegate and Simplify: This is not the time to be a hero. Order groceries online, let the laundry sit, and ask your partner to handle dinner. Conserve your energy for what truly matters: growing your baby.
3. The Essential Nutrition & Lifestyle Shift
What you do (and don’t do) now sets the stage for a healthy pregnancy.
- The Prenatal Vitamin Non-Negotiable: The most crucial ingredients are 400-800 mcg of folic acid (to prevent neural tube defects) and iron. DHA is a bonus for baby’s brain development. If pills worsen nausea, try taking them at night or ask your doctor about chewable or gummy options.
- Foods to Avoid When Newly Pregnant: This list is about avoiding bacteria and toxins that can harm your developing baby. Steer clear of: unpasteurized dairy/cheeses, raw or undercooked meat/seafood/eggs, deli meats unless heated steaming hot, high-mercury fish (shark, swordfish), and unpasteurized juices. When in doubt, heat it thoroughly or leave it out.
- Safe Exercises During First Trimester: Unless your doctor advises otherwise, continuing your pre-pregnancy routine is generally safe. Walking, swimming, prenatal yoga, and stationary cycling are fantastic. The goal is maintenance, not personal bests. Listen to your body—if something feels off, stop. Stay hydrated and avoid activities with a high risk of falling or abdominal impact.
Your Healthcare Partnership: The First Prenatal Visit
When to schedule your first prenatal visit is a common question. Most providers will see you between 8 and 10 weeks pregnant. This timing allows them to confirm a viable pregnancy with a heartbeat via ultrasound.
What to Expect at That First Appointment: Be prepared for a comprehensive visit. They’ll take a full medical history, perform a physical exam, and likely run a panel of blood tests (checking blood type, iron levels, immunity to certain diseases). You’ll also have a pelvic exam and possibly that first thrilling ultrasound. Come with a list of questions—no query is too small. This is the time to discuss your symptoms, medications, and any concerns about coping with pregnancy anxiety.
Partnering Through the Process: You’re Not Alone
This journey, while happening within your body, impacts your partner too. Communication is everything.
- Share the Information: Have them read this guide or parts of it. They may not understand why you’re exhausted at 7 PM or repulsed by a food you loved last week.
- Assign Concrete Tasks: Instead of “help more,” ask for specific things: “Could you be in charge of making sure we always have saltines and ginger ale?” or “I need you to handle the cat litter for the next few months.”
- Connect Beyond Symptoms: Schedule a weekly “non-pregnancy check-in.” Take a gentle walk or watch a funny movie. Remember, you are partners first, parents-to-be second.
Final Encouragement as You Finish the First Chapter
As you approach week 12, know that you are accomplishing something extraordinary. Every wave of nausea, every nap taken, every healthy choice is a testament to your strength and dedication to your baby. The second trimester often brings renewed energy and the joyful prospect of feeling those first flutters of movement.
You are not just surviving; you are laying the most perfect, loving foundation. Trust your body, partner with your care provider, and be gentle with yourself. You’ve got this.
Your First Trimester FAQ: Quick, Reassuring Answers
Q: Is it normal to have cramps in the first trimester?
A: Yes, mild, period-like cramps are very common as your uterus stretches and grows. However, severe, sharp, or persistent cramping accompanied by bleeding should prompt a call to your doctor.
Q: I have no morning sickness. Does that mean something is wrong?
A: Not at all! An estimated 20-30% of women experience little to no nausea. Consider yourself one of the lucky ones and try not to add worry to your plate.
Q: Can I still drink coffee?
A: Most experts agree that up to 200mg of caffeine per day (about one 12-oz cup of coffee) is considered safe during pregnancy. It’s about moderation.
Q: How do I deal with food aversions when I need to eat healthy?
A: Don’t fight them. Focus on what you can tolerate, even if it’s simple carbs for a short period. Prenatal vitamins will cover your nutritional bases. As your aversions ease (often in the second trimester), you can gradually reintroduce a wider variety of foods.
Q: When will I start to show?
A: Most first-time moms notice a small bump between 12 and 16 weeks. You might simply feel bloated before then. Everyone’s body is different!